Thank you for visiting nature.com. You are using a browser version with limited support for CSS. To obtain the best experience, we recommend you use a more up to date browser (or turn off compatibility mode in Internet Explorer). In the meantime, to ensure continued support, we are displaying the site without styles and JavaScript.
- View all journals
- Explore content
- About the journal
- Publish with us
- Sign up for alerts
- Perspective
- Open access
- Published: 16 October 2014

A woman with asthma: a whole systems approach to supporting self-management
- Hilary Pinnock 1 ,
- Elisabeth Ehrlich 1 ,
- Gaylor Hoskins 2 &
- Ron Tomlins 3
npj Primary Care Respiratory Medicine volume 24 , Article number: 14063 ( 2014 ) Cite this article
16k Accesses
2 Citations
6 Altmetric
Metrics details
- Health care
A 35-year-old lady attends for review of her asthma following an acute exacerbation. There is an extensive evidence base for supported self-management for people living with asthma, and international and national guidelines emphasise the importance of providing a written asthma action plan. Effective implementation of this recommendation for the lady in this case study is considered from the perspective of a patient, healthcare professional, and the organisation. The patient emphasises the importance of developing a partnership based on honesty and trust, the need for adherence to monitoring and regular treatment, and involvement of family support. The professional considers the provision of asthma self-management in the context of a structured review, with a focus on a self-management discussion which elicits the patient’s goals and preferences. The organisation has a crucial role in promoting, enabling and providing resources to support professionals to provide self-management. The patient’s asthma control was assessed and management optimised in two structured reviews. Her goal was to avoid disruption to her work and her personalised action plan focused on achieving that goal.
Similar content being viewed by others
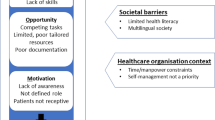
Barriers to implementing asthma self-management in Malaysian primary care: qualitative study exploring the perspectives of healthcare professionals

The self-management abilities test (SMAT): a tool to identify the self-management abilities of adults with bronchiectasis
Improving primary care management of asthma: do we know what really works?
A 35-year-old sales representative attends the practice for an asthma review. Her medical record notes that she has had asthma since childhood, and although for many months of the year her asthma is well controlled (when she often reduces or stops her inhaled steroids), she experiences one or two exacerbations a year requiring oral steroids. These are usually triggered by a viral upper respiratory infection, though last summer when the pollen count was particularly high she became tight chested and wheezy for a couple of weeks.
Her regular prescription is for fluticasone 100 mcg twice a day, and salbutamol as required. She has a young family and a busy lifestyle so does not often manage to find time to attend the asthma clinic. A few weeks previously, an asthma attack had interfered with some important work-related travel, and she has attended the clinic on this occasion to ask about how this can be managed better in the future. There is no record of her having been given an asthma action plan.
What do we know about asthma self-management? The academic perspective
Supported self-management reduces asthma morbidity.
The lady in this case study is struggling to maintain control of her asthma within the context of her busy professional and domestic life. The recent unfortunate experience which triggered this consultation offers a rare opportunity to engage with her and discuss how she can manage her asthma better. It behoves the clinician whom she is seeing (regardless of whether this is in a dedicated asthma clinic or an appointment in a routine general practice surgery) to grasp the opportunity and discuss self-management and provide her with a (written) personalised asthma action plan (PAAP).
The healthcare professional advising the lady is likely to be aware that international and national guidelines emphasise the importance of supporting self-management. 1 – 4 There is an extensive evidence base for asthma self-management: a recent synthesis identified 22 systematic reviews summarising data from 260 randomised controlled trials encompassing a broad range of demographic, clinical and healthcare contexts, which concluded that asthma self-management reduces emergency use of healthcare resources, including emergency department visits, hospital admissions and unscheduled consultations and improves markers of asthma control, including reduced symptoms and days off work, and improves quality of life. 1 , 2 , 5 – 12 Health economic analysis suggests that it is not only clinically effective, but also a cost-effective intervention. 13
Personalised asthma action plans
Key features of effective self-management approaches are:
Self-management education should be reinforced by provision of a (written) PAAP which reminds patients of their regular treatment, how to monitor and recognise that control is deteriorating and the action they should take. 14 – 16 As an adult, our patient can choose whether she wishes to monitor her control with symptoms or by recording peak flows (or a combination of both). 6 , 8 , 9 , 14 Symptom-based monitoring is generally better in children. 15 , 16
Plans should have between two and three action points including emergency doses of reliever medication; increasing low dose (or recommencing) inhaled steroids; or starting a course of oral steroids according to severity of the exacerbation. 14
Personalisation of the action plan is crucial. Focussing specifically on what actions she could take to prevent a repetition of the recent attack is likely to engage her interest. Not all patients will wish to start oral steroids without advice from a healthcare professional, though with her busy lifestyle and travel our patient is likely to be keen to have an emergency supply of prednisolone. Mobile technology has the potential to support self-management, 17 , 18 though a recent systematic review concluded that none of the currently available smart phone ‘apps’ were fit for purpose. 19
Identification and avoidance of her triggers is important. As pollen seems to be a trigger, management of allergic rhinitis needs to be discussed (and included in her action plan): she may benefit from regular use of a nasal steroid spray during the season. 20
Self-management as recommended by guidelines, 1 , 2 focuses narrowly on adherence to medication/monitoring and the early recognition/remediation of exacerbations, summarised in (written) PAAPs. Patients, however, may want to discuss how to reduce the impact of asthma on their life more generally, 21 including non-pharmacological approaches.
Supported self-management
The impact is greater if self-management education is delivered within a comprehensive programme of accessible, proactive asthma care, 22 and needs to be supported by ongoing regular review. 6 With her busy lifestyle, our patient may be reluctant to attend follow-up appointments, and once her asthma is controlled it may be possible to make convenient arrangements for professional review perhaps by telephone, 23 , 24 or e-mail. Flexible access to professional advice (e.g., utilising diverse modes of consultation) is an important component of supporting self-management. 25
The challenge of implementation
Implementation of self-management, however, remains poor in routine clinical practice. A recent Asthma UK web-survey estimated that only 24% of people with asthma in the UK currently have a PAAP, 26 with similar figures from Sweden 27 and Australia. 28 The general practitioner may feel that they do not have time to discuss self-management in a routine surgery appointment, or may not have a supply of paper-based PAAPs readily available. 29 However, as our patient rarely finds time to attend the practice, inviting her to make an appointment for a future clinic is likely to be unsuccessful and the opportunity to provide the help she needs will be missed.
The solution will need a whole systems approach
A systematic meta-review of implementing supported self-management in long-term conditions (including asthma) concluded that effective implementation was multifaceted and multidisciplinary; engaging patients, training and motivating professionals within the context of an organisation which actively supported self-management. 5 This whole systems approach considers that although patient education, professional training and organisational support are all essential components of successful support, they are rarely effective in isolation. 30 A systematic review of interventions that promote provision/use of PAAPs highlighted the importance of organisational systems (e.g., sending blank PAAPs with recall reminders). 31 A patient offers her perspective ( Box 1 ), a healthcare professional considers the clinical challenge, and the challenges are discussed from an organisational perspective.
Box 1: What self-management help should this lady expect from her general practitioner or asthma nurse? The patient’s perspective
The first priority is that the patient is reassured that her condition can be managed successfully both in the short and the long term. A good working relationship with the health professional is essential to achieve this outcome. Developing trust between patient and healthcare professional is more likely to lead to the patient following the PAAP on a long-term basis.
A review of all medication and possible alternative treatments should be discussed. The patient needs to understand why any changes are being made and when she can expect to see improvements in her condition. Be honest, as sometimes it will be necessary to adjust dosages before benefits are experienced. Be positive. ‘There are a number of things we can do to try to reduce the impact of asthma on your daily life’. ‘Preventer treatment can protect against the effect of pollen in the hay fever season’. If possible, the same healthcare professional should see the patient at all follow-up appointments as this builds trust and a feeling of working together to achieve the aim of better self-management.
Is the healthcare professional sure that the patient knows how to take her medication and that it is taken at the same time each day? The patient needs to understand the benefit of such a routine. Medication taken regularly at the same time each day is part of any self-management regime. If the patient is unused to taking medication at the same time each day then keeping a record on paper or with an electronic device could help. Possibly the patient could be encouraged to set up a system of reminders by text or smartphone.
Some people find having a peak flow meter useful. Knowing one's usual reading means that any fall can act as an early warning to put the PAAP into action. Patients need to be proactive here and take responsibility.
Ongoing support is essential for this patient to ensure that she takes her medication appropriately. Someone needs to be available to answer questions and provide encouragement. This could be a doctor or a nurse or a pharmacist. Again, this is an example of the partnership needed to achieve good asthma control.
It would also be useful at a future appointment to discuss the patient’s lifestyle and work with her to reduce her stress. Feeling better would allow her to take simple steps such as taking exercise. It would also be helpful if all members of her family understood how to help her. Even young children can do this.
From personal experience some people know how beneficial it is to feel they are in a partnership with their local practice and pharmacy. Being proactive produces dividends in asthma control.
What are the clinical challenges for the healthcare professional in providing self-management support?
Due to the variable nature of asthma, a long-standing history may mean that the frequency and severity of symptoms, as well as what triggers them, may have changed over time. 32 Exacerbations requiring oral steroids, interrupting periods of ‘stability’, indicate the need for re-assessment of the patient’s clinical as well as educational needs. The patient’s perception of stability may be at odds with the clinical definition 1 , 33 —a check on the number of short-acting bronchodilator inhalers the patient has used over a specific period of time is a good indication of control. 34 Assessment of asthma control should be carried out using objective tools such as the Asthma Control Test or the Royal College of Physicians three questions. 35 , 36 However, it is important to remember that these assessment tools are not an end in themselves but should be a springboard for further discussion on the nature and pattern of symptoms. Balancing work with family can often make it difficult to find the time to attend a review of asthma particularly when the patient feels well. The practice should consider utilising other means of communication to maintain contact with patients, encouraging them to come in when a problem is highlighted. 37 , 38 Asthma guidelines advocate a structured approach to ensure the patient is reviewed regularly and recommend a detailed assessment to enable development of an appropriate patient-centred (self)management strategy. 1 – 4
Although self-management plans have been shown to be successful for reducing the impact of asthma, 21 , 39 the complexity of managing such a fluctuating disease on a day-to-day basis is challenging. During an asthma review, there is an opportunity to work with the patient to try to identify what triggers their symptoms and any actions that may help improve or maintain control. 38 An integral part of personalised self-management education is the written PAAP, which gives the patient the knowledge to respond to the changes in symptoms and ensures they maintain control of their asthma within predetermined parameters. 9 , 40 The PAAP should include details on how to monitor asthma, recognise symptoms, how to alter medication and what to do if the symptoms do not improve. The plan should include details on the treatment to be taken when asthma is well controlled, and how to adjust it when the symptoms are mild, moderate or severe. These action plans need to be developed between the doctor, nurse or asthma educator and the patient during the review and should be frequently reviewed and updated in partnership (see Box 1). Patient preference as well as clinical features such as whether she under- or over-perceives her symptoms should be taken into account when deciding whether the action plan is peak flow or symptom-driven. Our patient has a lot to gain from having an action plan. She has poorly controlled asthma and her lifestyle means that she will probably see different doctors (depending who is available) when she needs help. Being empowered to self-manage could make a big difference to her asthma control and the impact it has on her life.
The practice should have protocols in place, underpinned by specific training to support asthma self-management. As well as ensuring that healthcare professionals have appropriate skills, this should include training for reception staff so that they know what action to take if a patient telephones to say they are having an asthma attack.
However, focusing solely on symptom management strategies (actions) to follow in the presence of deteriorating symptoms fails to incorporate the patients’ wider views of asthma, its management within the context of her/his life, and their personal asthma management strategies. 41 This may result in a failure to use plans to maximise their health potential. 21 , 42 A self-management strategy leading to improved outcomes requires a high level of patient self-efficacy, 43 a meaningful partnership between the patient and the supporting health professional, 42 , 44 and a focused self-management discussion. 14
Central to both the effectiveness and personalisation of action plans, 43 , 45 in particular the likelihood that the plan will lead to changes in patients’ day-to-day self-management behaviours, 45 is the identification of goals. Goals are more likely to be achieved when they are specific, important to patients, collaboratively set and there is a belief that these can be achieved. Success depends on motivation 44 , 46 to engage in a specific behaviour to achieve a valued outcome (goal) and the ability to translate the behavioural intention into action. 47 Action and coping planning increases the likelihood that patient behaviour will actually change. 44 , 46 , 47 Our patient has a goal: she wants to avoid having her work disrupted by her asthma. Her personalised action plan needs to explicitly focus on achieving that goal.
As providers of self-management support, health professionals must work with patients to identify goals (valued outcomes) that are important to patients, that may be achievable and with which they can engage. The identification of specific, personalised goals and associated feasible behaviours is a prerequisite for the creation of asthma self-management plans. Divergent perceptions of asthma and how to manage it, and a mismatch between what patients want/need from these plans and what is provided by professionals are barriers to success. 41 , 42
What are the challenges for the healthcare organisation in providing self-management support?
A number of studies have demonstrated the challenges for primary care physicians in providing ongoing support for people with asthma. 31 , 48 , 49 In some countries, nurses and other allied health professionals have been trained as asthma educators and monitor people with stable asthma. These resources are not always available. In addition, some primary care services are delivered in constrained systems where only a few minutes are available to the practitioner in a consultation, or where only a limited range of asthma medicines are available or affordable. 50
There is recognition that the delivery of quality care depends on the competence of the doctor (and supporting health professionals), the relationship between the care providers and care recipients, and the quality of the environment in which care is delivered. 51 This includes societal expectations, health literacy and financial drivers.
In 2001, the Australian Government adopted a programme developed by the General Practitioner Asthma Group of the National Asthma Council Australia that provided a structured approach to the implementation of asthma management guidelines in a primary care setting. 52 Patients with moderate-to-severe asthma were eligible to participate. The 3+ visit plan required confirmation of asthma diagnosis, spirometry if appropriate, assessment of trigger factors, consideration of medication and patient self-management education including provision of a written PAAP. These elements, including regular medical review, were delivered over three visits. Evaluation demonstrated that the programme was beneficial but that it was difficult to complete the third visit in the programme. 53 – 55 Accordingly, the programme, renamed the Asthma Cycle of Care, was modified to incorporate two visits. 56 Financial incentives are provided to practices for each patient who receives this service each year.
Concurrently, other programmes were implemented which support practice-based care. Since 2002, the National Asthma Council has provided best-practice asthma and respiratory management education to health professionals, 57 and this programme will be continuing to 2017. The general practitioner and allied health professional trainers travel the country to provide asthma and COPD updates to groups of doctors, nurses and community pharmacists. A number of online modules are also provided. The PACE (Physician Asthma Care Education) programme developed by Noreen Clark has also been adapted to the Australian healthcare system. 58 In addition, a pharmacy-based intervention has been trialled and implemented. 59
To support these programmes, the National Asthma Council ( www.nationalasthma.org.au ) has developed resources for use in practices. A strong emphasis has been on the availability of a range of PAAPs (including plans for using adjustable maintenance dosing with ICS/LABA combination inhalers), plans for indigenous Australians, paediatric plans and plans translated into nine languages. PAAPs embedded in practice computer systems are readily available in consultations, and there are easily accessible online paediatric PAAPs ( http://digitalmedia.sahealth.sa.gov.au/public/asthma/ ). A software package, developed in the UK, can be downloaded and used to generate a pictorial PAAP within the consultation. 60
One of the strongest drivers towards the provision of written asthma action plans in Australia has been the Asthma Friendly Schools programme. 61 , 62 Established with Australian Government funding and the co-operation of Education Departments of each state, the Asthma Friendly Schools programme engages schools to address and satisfy a set of criteria that establishes an asthma-friendly environment. As part of accreditation, the school requires that each child with asthma should have a written PAAP prepared by their doctor to assist (trained) staff in managing a child with asthma at school.
The case study continues...
The initial presentation some weeks ago was during an exacerbation of asthma, which may not be the best time to educate a patient. It is, however, a splendid time to build on their motivation to feel better. She agreed to return after her asthma had settled to look more closely at her asthma control, and an appointment was made for a routine review.
At this follow-up consultation, the patient’s diagnosis was reviewed and confirmed and her trigger factors discussed. For this lady, respiratory tract infections are the usual trigger but allergic factors during times of high pollen count may also be relevant. Assessment of her nasal airway suggested that she would benefit from better control of allergic rhinitis. Other factors were discussed, as many patients are unaware that changes in air temperature, exercise and pets can also trigger asthma exacerbations. In addition, use of the Asthma Control Test was useful as an objective assessment of control as well as helping her realise what her life could be like! Many people with long-term asthma live their life within the constraints of their illness, accepting that is all that they can do.
After assessing the level of asthma control, a discussion about management options—trigger avoidance, exercise and medicines—led to the development of a written PAAP. Asthma can affect the whole family, and ways were explored that could help her family understand why it is important that she finds time in the busy domestic schedules to take her regular medication. Family and friends can also help by understanding what triggers her asthma so that they can avoid exposing her to perfumes, pollens or pets that risk triggering her symptoms. Information from the national patient organisation was provided to reinforce the messages.
The patient agreed to return in a couple of weeks, and a recall reminder was set up. At the second consultation, the level of control since the last visit will be explored including repeat spirometry, if appropriate. Further education about the pathophysiology of asthma and how to recognise early warning signs of loss of control can be given. Device use will be reassessed and the PAAP reviewed. Our patient’s goal is to avoid disruption to her work and her PAAP will focus on achieving that goal. Finally, agreement will be reached with the patient about future routine reviews, which, now that she has a written PAAP, could be scheduled by telephone if all is well, or face-to-face if a change in her clinical condition necessitates a more comprehensive review.
Global Initiative for Asthma. Global Strategy for Asthma Management and Prevention, 2012. Available from: http://www.ginasthma.org (accessed July 2013).
British Thoracic Society/Scottish Intercollegiate Guideline Network British Guideline on the Management of Asthma. Thorax 2008; 63 (Suppl 4 iv1–121, updated version available from: http://www.sign.ac.uk (accessed January 2014).
Article Google Scholar
National Asthma Council Australia. Australian Asthma Handbook. Available from: http://www.nationalasthma.org.au/handbook (accessed May 2014).
National Asthma Education and Prevention Program (NAEPP) Coordinating Committee. Expert Panel Report 3 (EPR3): Guidelines for the Diagnosis and Management of Asthma. Available from: https://www.nhlbi.nih.gov/guidelines/asthma/asthgdln.htm (accessed May 2014).
Taylor SJC, Pinnock H, Epiphaniou E, Pearce G, Parke H . A rapid synthesis of the evidence on interventions supporting self-management for people with long-term conditions. (PRISMS Practical Systematic Review of Self-Management Support for long-term conditions). Health Serv Deliv Res (in press).
Gibson PG, Powell H, Wilson A, Abramson MJ, Haywood P, Bauman A et al. Self-management education and regular practitioner review for adults with asthma. Cochrane Database Syst Rev 2002: (Issue 3) Art No. CD001117.
Tapp S, Lasserson TJ, Rowe BH . Education interventions for adults who attend the emergency room for acute asthma. Cochrane Database Syst Rev 2007: (Issue 3) Art No. CD003000.
Powell H, Gibson PG . Options for self-management education for adults with asthma. Cochrane Database Syst Rev 2002: (Issue 3) Art No: CD004107.
Toelle B, Ram FSF . Written individualised management plans for asthma in children and adults. Cochrane Database Syst Rev 2004: (Issue 1) Art No. CD002171.
Lefevre F, Piper M, Weiss K, Mark D, Clark N, Aronson N . Do written action plans improve patient outcomes in asthma? An evidence-based analysis. J Fam Pract 2002; 51 : 842–848.
PubMed Google Scholar
Boyd M, Lasserson TJ, McKean MC, Gibson PG, Ducharme FM, Haby M . Interventions for educating children who are at risk of asthma-related emergency department attendance. Cochrane Database Syst Rev 2009: (Issue 2) Art No.CD001290.
Bravata DM, Gienger AL, Holty JE, Sundaram V, Khazeni N, Wise PH et al. Quality improvement strategies for children with asthma: a systematic review. Arch Pediatr Adolesc Med 2009; 163 : 572–581.
Bower P, Murray E, Kennedy A, Newman S, Richardson G, Rogers A . Self-management support interventions to reduce health care utilisation without compromising outcomes: a rapid synthesis of the evidence. Available from: http://www.nets.nihr.ac.uk/projects/hsdr/11101406 (accessed April 2014).
Gibson PG, Powell H . Written action plans for asthma: an evidence-based review of the key components. Thorax 2004; 59 : 94–99.
Article CAS Google Scholar
Bhogal SK, Zemek RL, Ducharme F . Written action plans for asthma in children. Cochrane Database Syst Rev 2006: (Issue 3) Art No. CD005306.
Zemek RL, Bhogal SK, Ducharme FM . Systematic review of randomized controlled trials examining written action plans in children: what is the plan?. Arch Pediatr Adolesc Med 2008; 162 : 157–163.
Pinnock H, Slack R, Pagliari C, Price D, Sheikh A . Understanding the potential role of mobile phone based monitoring on asthma self-management: qualitative study. Clin Exp Allergy 2007; 37 : 794–802.
de Jongh T, Gurol-Urganci I, Vodopivec-Jamsek V, Car J, Atun R . Mobile phone messaging for facilitating self-management of long-term illnesses. Cochrane Database Syst Rev 2012: (Issue 12) Art No. CD007459.
Huckvale K, Car M, Morrison C, Car J . Apps for asthma self-management: a systematic assessment of content and tools. BMC Med 2012; 10 : 144.
Allergic Rhinitis and its Impact on Asthma. Management of Allergic Rhinitis and its Impact on Asthma: Pocket Guide. ARIA 2008. Available from: http://www.whiar.org (accessed May 2014).
Ring N, Jepson R, Hoskins G, Wilson C, Pinnock H, Sheikh A et al. Understanding what helps or hinders asthma action plan use: a systematic review and synthesis of the qualitative literature. Patient Educ Couns 2011; 85 : e131–e143.
Moullec G, Gour-Provencal G, Bacon SL, Campbell TS, Lavoie KL . Efficacy of interventions to improve adherence to inhaled corticosteroids in adult asthmatics: Impact of using components of the chronic care model. Respir Med 2012; 106 : 1211–1225.
Pinnock H, Bawden R, Proctor S, Wolfe S, Scullion J, Price D et al. Accessibility, acceptability and effectiveness of telephone reviews for asthma in primary care: randomised controlled trial. BMJ 2003; 326 : 477–479.
Pinnock H, Adlem L, Gaskin S, Harris J, Snellgrove C, Sheikh A . Accessibility, clinical effectiveness and practice costs of providing a telephone option for routine asthma reviews: phase IV controlled implementation study. Br J Gen Pract 2007; 57 : 714–722.
PubMed PubMed Central Google Scholar
Kielmann T, Huby G, Powell A, Sheikh A, Price D, Williams S et al. From support to boundary: a qualitative study of the border between self care and professional care. Patient Educ Couns 2010; 79 : 55–61.
Asthma UK . Compare your care report. Asthma UK, 2013. Available from: http://www.asthma.org.uk (accessed January 2014).
Stallberg B, Lisspers K, Hasselgren M, Janson C, Johansson G, Svardsudd K . Asthma control in primary care in Sweden: a comparison between 2001 and 2005. Prim Care Respir J 2009; 18 : 279–286.
Reddel H, Peters M, Everett P, Flood P, Sawyer S . Ownership of written asthma action plans in a large Australian survey. Eur Respir J 2013; 42 . Abstract 2011.
Wiener-Ogilvie S, Pinnock H, Huby G, Sheikh A, Partridge MR, Gillies J . Do practices comply with key recommendations of the British Asthma Guideline? If not, why not? Prim Care Respir J 2007; 16 : 369–377.
Kennedy A, Rogers A, Bower P . Support for self care for patients with chronic disease. BMJ 2007; 335 : 968–970.
Ring N, Malcolm C, Wyke S, Macgillivray S, Dixon D, Hoskins G et al. Promoting the Use of Personal Asthma Action Plans: A Systematic Review. Prim Care Respir J 2007; 16 : 271–283.
Taylor DR, Bateman ED, Boulet LP, Boushey HA, Busse WW, Casale TB et al. A new perspective on concepts of asthma severity and control. Eur Respir J 2008; 32 : 545–554.
Horne R . Compliance, adherence, and concordance: implications for asthma treatment. Chest 2006; 130 (suppl): 65S–72S.
Reddel HK, Taylor DR, Bateman ED, Boulet L-P, Boushey HA, Busse WW et al. An official American Thoracic Society/European Respiratory Society statement: asthma control and exacerbations standardizing endpoints for clinical asthma trials and clinical practice. Am J Respir Crit Care Med 2009; 180 : 59–99.
Thomas M, Kay S, Pike J, Rosenzweig JR, Hillyer EV, Price D . The Asthma Control Test (ACT) as a predictor of GINA guideline-defined asthma control: analysis of a multinational cross-sectional survey. Prim Care Respir J 2009; 18 : 41–49.
Hoskins G, Williams B, Jackson C, Norman P, Donnan P . Assessing asthma control in UK primary care: use of routinely collected prospective observational consultation data to determine appropriateness of a variety of control assessment models. BMC Fam Pract 2011; 12 : 105.
Pinnock H, Fletcher M, Holmes S, Keeley D, Leyshon J, Price D et al. Setting the standard for routine asthma consultations: a discussion of the aims, process and outcomes of reviewing people with asthma in primary care. Prim Care Respir J 2010; 19 : 75–83.
McKinstry B, Hammersley V, Burton C, Pinnock H, Elton RA, Dowell J et al. The quality, safety and content of telephone and face-to-face consultations: a comparative study. Qual Saf Health Care 2010; 19 : 298–303.
Gordon C, Galloway T . Review of Findings on Chronic Disease Self-Management Program (CDSMP) Outcomes: Physical, Emotional & Health-Related Quality of Life, Healthcare Utilization and Costs . Centers for Disease Control and Prevention and National Council on Aging: Atlanta, GA, USA, 2008.
Beasley R, Crane J . Reducing asthma mortality with the self-management plan system of care. Am J Respir Crit Care Med 2001; 163 : 3–4.
Ring N, Jepson R, Pinnock H, Wilson C, Hoskins G, Sheikh A et al. Encouraging the promotion and use of asthma action plans: a cross study synthesis of qualitative and quantitative evidence. Trials 2012; 13 : 21.
Jones A, Pill R, Adams S . Qualitative study of views of health professionals and patients on guided self-management plans for asthma. BMJ 2000; 321 : 1507–1510.
Bandura A . Self-efficacy: toward a unifying theory of behavioural change. Psychol Rev 1977; 84 : 191–215.
Gollwitzer PM, Sheeran P . Implementation intentions and goal achievement: a meta-analysis of effects and processes. Adv Exp Soc Psychol 2006; 38 : 69–119.
Google Scholar
Hardeman W, Johnston M, Johnston DW, Bonetti D, Wareham NJ, Kinmonth AL . Application of the theory of planned behaviour change interventions: a systematic review. Psychol Health 2002; 17 : 123–158.
Schwarzer R . Modeling health behavior change: how to predict and modify the adoption and maintenance of health behaviors. Appl Psychol 2008; 57 : 1–29.
Sniehotta F . Towards a theory of intentional behaviour change: plans, planning, and self-regulation. Br J Health Psychol 2009; 14 : 261–273.
Okelo SO, Butz AM, Sharma R, Diette GB, Pitts SI, King TM et al. Interventions to modify health care provider adherence to asthma guidelines: a systematic review. Pediatrics 2013; 132 : 517–534.
Grol R, Grimshaw RJ . From best evidence to best practice: effective implementation of change in patients care. Lancet 2003; 362 : 1225–1230.
Jusef L, Hsieh C-T, Abad L, Chaiyote W, Chin WS, Choi Y-J et al. Primary care challenges in treating paediatric asthma in the Asia-Pacific region. Prim Care Respir J 2013; 22 : 360–362.
Donabedian A . Evaluating the quality of medical care. Milbank Q 2005; 83 : 691–729.
Fardy HJ . Moving towards organized care of chronic disease. The 3+ visit plan. Aust Fam Physician 2001; 30 : 121–125.
CAS PubMed Google Scholar
Glasgow NJ, Ponsonby AL, Yates R, Beilby J, Dugdale P . Proactive asthma care in childhood: general practice based randomised controlled trial. BMJ 2003; 327 : 659.
Douglass JA, Goemann DP, Abramson MJ . Asthma 3+ visit plan: a qualitative evaluation. Intern Med J 2005; 35 : 457–462.
Beilby J, Holton C . Chronic disease management in Australia; evidence and policy mismatch, with asthma as an example. Chronic Illn 2005; 1 : 73–80.
The Department of Health. Asthma Cycle of Care. Accessed on 14 May 2014 at http://www.health.gov.au/internet/main/publishing.nsf/Content/asthma-cycle .
National Asthma Council Australia. Asthma and Respiratory Education Program. Accessed on 14 May 2014 at http://www.nationalasthma.org.au/health-professionals/education-training/asthma-respiratory-education-program .
Patel MR, Shah S, Cabana MD, Sawyer SM, Toelle B, Mellis C et al. Translation of an evidence-based asthma intervention: Physician Asthma Care Education (PACE) in the United States and Australia. Prim Care Respir J 2013; 22 : 29–34.
Armour C, Bosnic-Anticevich S, Brilliant M, Burton D, Emmerton L, Krass I et al. Pharmacy Asthma Care Program (PACP) improves outcomes for patients in the community. Thorax 2007; 62 : 496–502.
Roberts NJ, Mohamed Z, Wong PS, Johnson M, Loh LC, Partridge MR . The development and comprehensibility of a pictorial asthma action plan. Patient Educ Couns 2009; 74 : 12–18.
Henry RL, Gibson PG, Vimpani GV, Francis JL, Hazell J . Randomised controlled trial of a teacher-led asthma education program. Pediatr Pulmonol 2004; 38 : 434–442.
National Asthma Council Australia. Asthma Friendly Schools program. Accessed on 14 May 2014 at http://www.asthmaaustralia.org.au/Asthma-Friendly-Schools.aspx .
Download references
Author information
Authors and affiliations.
Asthma UK Centre for Applied Research, Centre for Population Health Sciences, The University of Edinburgh, Edinburgh, UK,
Hilary Pinnock & Elisabeth Ehrlich
NMAHP-RU, University of Stirling, Stirling, UK,
Gaylor Hoskins
Discipline of General Practice, University of Sydney, Sydney, NSW, Australia
Ron Tomlins
You can also search for this author in PubMed Google Scholar
Corresponding author
Correspondence to Hilary Pinnock .
Ethics declarations
Competing interests.
The authors declare no conflict of interest.
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License. The images or other third party material in this article are included in the article's Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/4.0/
Reprints and permissions
About this article
Cite this article.
Pinnock, H., Ehrlich, E., Hoskins, G. et al. A woman with asthma: a whole systems approach to supporting self-management. npj Prim Care Resp Med 24 , 14063 (2014). https://doi.org/10.1038/npjpcrm.2014.63
Download citation
Received : 23 June 2014
Revised : 15 July 2014
Accepted : 15 July 2014
Published : 16 October 2014
DOI : https://doi.org/10.1038/npjpcrm.2014.63
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
Quick links
- Explore articles by subject
- Guide to authors
- Editorial policies
Sign up for the Nature Briefing newsletter — what matters in science, free to your inbox daily.
Case Study: Managing Severe Asthma in an Adult
—he follows his treatment plan, but this 40-year-old male athlete has asthma that is not well-controlled. what’s the next step.
By Kirstin Bass, MD, PhD Reviewed by Michael E. Wechsler, MD, MMSc
This case presents a patient with poorly controlled asthma that remains refractory to treatment despite use of standard-of-care therapeutic options. For patients such as this, one needs to embark on an extensive work-up to confirm the diagnosis, assess for comorbidities, and finally, to consider different therapeutic options.

Case presentation and patient history
Mr. T is a 40-year-old recreational athlete with a medical history significant for asthma, for which he has been using an albuterol rescue inhaler approximately 3 times per week for the past year. During this time, he has also been waking up with asthma symptoms approximately twice a month, and has had three unscheduled asthma visits for mild flares. Based on the National Asthma Education and Prevention Program guidelines , Mr. T has asthma that is not well controlled. 1
As a result of these symptoms, spirometry was performed revealing a forced expiratory volume in the first second (FEV1) of 78% predicted. Mr. T then was prescribed treatment with a low-dose corticosteroid, fluticasone 44 mcg at two puffs twice per day. However, he remained symptomatic and continued to use his rescue inhaler 3 times per week. Therefore, he was switched to a combination inhaled steroid and long-acting beta-agonist (LABA) (fluticasone propionate 250 mcg and salmeterol 50 mcg, one puff twice a day) by his primary care doctor.
Initial pulmonary assessment Even with this step up in his medication, Mr. T continued to be symptomatic and require rescue inhaler use. Therefore, he was referred to a pulmonologist, who performed the initial work-up shown here:
- Spirometry, pre-albuterol: FEV1 79%, post-albuterol: 12% improvement
- Methacholine challenge: PC 20 : 1.0 mg/mL
- Chest X-ray: Within normal limits
Continued pulmonary assessment His dose of inhaled corticosteroid (ICS) and LABA was increased to fluticasone 500 mcg/salmeterol 50 mcg, one puff twice daily. However, he continued to have symptoms and returned to the pulmonologist for further work-up, shown here:
- Chest computed tomography (CT): Normal lung parenchyma with no scarring or bronchiectasis
- Sinus CT: Mild mucosal thickening
- Complete blood count (CBC): Within normal limits, white blood cells (WBC) 10.0 K/mcL, 3% eosinophils
- Immunoglobulin E (IgE): 25 IU/mL
- Allergy-skin test: Positive for dust, trees
- Exhaled NO: Fractional exhaled nitric oxide (FeNO) 53 parts per billion (pbb)
Assessment for comorbidities contributing to asthma symptoms After this work-up, tiotropium was added to his medication regimen. However, he remained symptomatic and had two more flares over the next 3 months. He was assessed for comorbid conditions that might be affecting his symptoms, and results showed:
- Esophagram/barium swallow: Negative
- Esophageal manometry: Negative
- Esophageal impedance: Within normal limits
- ECG: Within normal limits
- Genetic testing: Negative for cystic fibrosis, alpha1 anti-trypsin deficiency
The ear, nose, and throat specialist to whom he was referred recommended only nasal inhaled steroids for his mild sinus disease and noted that he had a normal vocal cord evaluation.
Following this extensive work-up that transpired over the course of a year, Mr. T continued to have symptoms. He returned to the pulmonologist to discuss further treatment options for his refractory asthma.
Diagnosis Mr. T has refractory asthma. Work-up for this condition should include consideration of other causes for the symptoms, including allergies, gastroesophageal reflux disease, cardiac disease, sinus disease, vocal cord dysfunction, or genetic diseases, such as cystic fibrosis or alpha1 antitrypsin deficiency, as was performed for Mr. T by his pulmonary team.
Treatment options When a patient has refractory asthma, treatment options to consider include anticholinergics (tiotropium, aclidinium), leukotriene modifiers (montelukast, zafirlukast), theophylline, anti-immunoglobulin E (IgE) antibody therapy with omalizumab, antibiotics, bronchial thermoplasty, or enrollment in a clinical trial evaluating the use of agents that modulate the cell signaling and immunologic responses seen in asthma.
Treatment outcome Mr. T underwent bronchial thermoplasty for his asthma. One year after the procedure, he reports feeling great. He has not taken systemic steroids for the past year, and his asthma remains controlled on a moderate dose of ICS and a LABA. He has also been able to resume exercising on a regular basis.
Approximately 10% to 15% of asthma patients have severe asthma refractory to the commonly available medications. 2 One key aspect of care for this patient population is a careful workup to exclude other comorbidities that could be contributing to their symptoms. Following this, there are several treatment options to consider, as in recent years there have been several advances in the development of asthma therapeutics. 2
Treatment options for refractory asthma There are a number of currently approved therapies for severe, refractory asthma. In addition to therapy with ICS or combination therapies with ICS and LABAs, leukotriene antagonists have good efficacy in asthma, especially in patients with prominent allergic or exercise symptoms. 2 The anticholinergics, such as tiotropium, which was approved for asthma in 2015, enhance bronchodilation and are useful adjuncts to ICS. 3-5 Omalizumab is a monoclonal antibody against IgE recommended for use in severe treatment-refractory allergic asthma in patients with atopy. 2 A nonmedication therapeutic option to consider is bronchial thermoplasty, a bronchoscopic procedure that uses thermal energy to disrupt bronchial smooth muscle. 6,7
Personalizing treatment for each patient It is important to personalize treatment based on individual characteristics or phenotypes that predict the patient's likely response to treatment, as well as the patient's preferences and practical issues, such as adherence and cost. 8
In this case, tiotropium had already been added to Mr. T's medications and his symptoms continued. Although addition of a leukotriene modifier was an option for him, he did not wish to add another medication to his care regimen. Omalizumab was not added partly for this reason, and also because of his low IgE level. As his bronchoscopy was negative, it was determined that a course of antibiotics would not be an effective treatment option for this patient. While vitamin D insufficiency has been associated with adverse outcomes in asthma, T's vitamin D level was tested and found to be sufficient.
We discussed the possibility of Mr. T's enrollment in a clinical trial. However, because this did not guarantee placement within a treatment arm and thus there was the possibility of receiving placebo, he opted to undergo bronchial thermoplasty.
Bronchial thermoplasty Bronchial thermoplasty is effective for many patients with severe persistent asthma, such as Mr. T. This procedure may provide additional benefits to, but does not replace, standard asthma medications. During the procedure, thermal energy is delivered to the airways via a bronchoscope to reduce excess airway smooth muscle and limit its ability to constrict the airways. It is an outpatient procedure performed over three sessions by a trained physician. 9
The effects of bronchial thermoplasty have been studied in several trials. The first large-scale multicenter randomized controlled study was the Asthma Intervention Research (AIR) Trial , which enrolled patients with moderate to severe asthma. 10 In this trial, patients who underwent the procedure had a significant improvement in asthma symptoms as measured by symptom-free days and scores on asthma control and quality of life questionnaires, as well as reductions in mild exacerbations and increases in morning peak expiratory flow. 10 Shortly after the AIR trial, the Research in Severe Asthma (RISA) trial was conducted to evaluate bronchial thermoplasty in patients with more severe, symptomatic asthma. 11 In this population, bronchial thermoplasty resulted in a transient worsening of asthma symptoms, with a higher rate of hospitalizations during the treatment period. 11 Hospitalization rate equalized between the treatment and control groups in the posttreatment period, however, and the treatment group showed significant improvements in rescue medication use, prebronchodilator forced expiratory volume in the first second (FEV1) % predicted, and asthma control questionnaire scores. 11
The AIR-2 trial followed, which was a multicenter, randomized, double-blind, sham-controlled study of 288 patients with severe asthma. 6 Similar to the RISA trial, patients in the treatment arm of this trial experienced an increase in adverse respiratory effects during the treatment period, the most common being airway irritation (including wheezing, chest discomfort, cough, and chest pain) and upper respiratory tract infections. 6
The majority of adverse effects occurred within 1 day of the procedure and resolved within 7 days. 6 In this study, bronchial thermoplasty was found to significantly improve quality of life, as well as reduce the rate of severe exacerbations by 32%. 6 Patients who underwent the procedure also reported fewer adverse respiratory effects, fewer days lost from work, school, or other activities due to asthma, and an 84% risk reduction in emergency department visits. 6
Long-term (5-year) follow-up studies have been conducted for patients in both the AIR and the AIR-2 trials. In patients who underwent bronchial thermoplasty in either study, the rate of adverse respiratory effects remained stable in years 2 to 5 following the procedure, with no increase in hospitalizations or emergency department visits. 7,12 Additionally, FEV1 remained stable throughout the 5-year follow-up period. 7,12 This finding was maintained in patients enrolled in the AIR-2 trial despite decreased use of daily ICS. 7
Bronchial thermoplasty is an important addition to the asthma treatment armamentarium. 7 This treatment is currently approved for individuals with severe persistent asthma who remain uncontrolled despite the use of an ICS and LABA. Several clinical trials with long-term follow-up have now demonstrated its safety and ability to improve quality of life in patients with severe asthma, such as Mr. T.
Severe asthma can be a challenge to manage. Patients with this condition require an extensive workup, but there are several treatments currently available to help manage these patients, and new treatments are continuing to emerge. Managing severe asthma thus requires knowledge of the options available as well as consideration of a patient's personal situation-both in terms of disease phenotype and individual preference. In this case, the patient expressed a strong desire to not add any additional medications to his asthma regimen, which explained the rationale for choosing to treat with bronchial thermoplasty. Personalized treatment necessitates exploring which of the available or emerging options is best for each individual patient.
Published: April 16, 2018
- 1. National Asthma Education and Prevention Program: Asthma Care Quick Reference.
- 2. Olin JT, Wechsler ME. Asthma: pathogenesis and novel drugs for treatment. BMJ . 2014;349:g5517.
- 3. Boehringer Ingelheim. Asthma: U.S. FDA approves new indication for SPIRIVA Respimat [press release]. September 16, 2015.
- 4. Peters SP, Kunselman SJ, Icitovic N, et al. Tiotropium bromide step-up therapy for adults with uncontrolled asthma. N Engl J Med . 2010;363:1715-1726.
- 5. Kerstjens HA, Engel M, Dahl R. Tiotropium in asthma poorly controlled with standard combination therapy. N Engl J Med . 2012;367:1198-1207.
- 6. Castro M, Rubin AS, Laviolette M, et al. Effectiveness and safety of bronchial thermoplasty in the treatment of severe asthma: a multicenter, randomized, double-blind, sham-controlled clinical trial. Am J Respir Crit Care Med . 2010;181:116-124.
- 7. Wechsler ME, Laviolette M, Rubin AS, et al. Bronchial thermoplasty: long-term safety and effectiveness in patients with severe persistent asthma. J Allergy Clin Immunol . 2013;132:1295-1302.
- 8. Global Initiative for Asthma: Pocket Guide for Asthma Management and Prevention (for Adults and Children Older than 5 Years).
- 10. Cox G, Thomson NC, Rubin AS, et al. Asthma control during the year after bronchial thermoplasty. N Engl J Med . 2007;356:1327-1337.
- 11. Pavord ID, Cox G, Thomson NC, et al. Safety and efficacy of bronchial thermoplasty in symptomatic, severe asthma. Am J Respir Crit Care Med . 2007;176:1185-1191.
- 12. Thomson NC, Rubin AS, Niven RM, et al. Long-term (5 year) safety of bronchial thermoplasty: Asthma Intervention Research (AIR) trial. BMC Pulm Med . 2011;11:8.
Treatable traits and future exacerbation risk in severe asthma, baker’s asthma, the long-term trajectory of mild asthma, age, gender, & systemic corticosteroid comorbidities, ask the expert: william busse, md, challenges the current definition of the atopic march, considering the curveballs in asthma treatment, do mucus plugs play a bigger role in chronic severe asthma than previously thought, an emerging subtype of copd is associated with early respiratory disease.

- Open access
- Published: 03 April 2020
Determinants of Acute Asthma Attack among adult asthmatic patients visiting hospitals of Tigray, Ethiopia, 2019: case control study
- Melaku Negash 1 ,
- Hagos Tsegabrhan 2 ,
- Teklit Meles 3 ,
- Degena Bahrey Tadesse 1 ,
- Gebreamlak Gidey 4 ,
- Yemane Berhane 5 ,
- Kibrom Berhanu 6 &
- Tsgalem Haylemaryam 7
Asthma Research and Practice volume 6 , Article number: 1 ( 2020 ) Cite this article
5093 Accesses
3 Citations
3 Altmetric
Metrics details
Introduction
Acute asthma attack is one of the most common causes of visits to hospital emergency departments in all age groups of the population and accounts for the greater part of healthcare burden from the disease. Despite, Acute asthma attack is an important public health problem that affects not only the patients, but also to the family, health professionals, health care institutions and development of the nation, little is known about the risk factors of acute asthma attack.
Therefore, this study is aimed to investigate the determinants of acute asthma attack among.
The aim of this study was to assess the determinant factors of acute asthma attack among adult asthmatic patients visiting general hospitals of central zone, Tigray, Ethiopia, 2019.
Hospital based unmatched case control study design was conducted in general hospitals of central zone of Tigray, Ethiopia 2019. Data were collected using pretested interviewer administered questionnaire. A total of 289 study subjects (96 cases &193 controls) were selected by systematic random sampling. Data were entered to Epi data version 3.1 then exported to SPSS version 23 for analysis. Bivariate logistic regression was employed to examine the statistical association between dependent and independent variables. Variables with p value < 0.25 in binary logistic regression were entered to multivariable logistic regression model and variables with p value < 0.05 was taken as significant determinants of the outcome variable.
A total of 96 adult asthmatic patients who have acute asthma attack (cases) and 193 adult asthmatic patients without attack (controls)) with 100% response rate were participated in this study. Upper Respiratory tract Infection [AOR = 6.835,95% CI = 3.285,14.222], Season [AOR =2.204,95% CI = 1.011,4.805] kitchen smoke [AOR = 2.307,95%CI1.010,5.272]& sleep apnea [AOR = 9.254, 5%CI =3.563,25.460] were significantly associated with acute asthma exacerbation.
Asthma is a long-term inflammatory disease of the respiratory system which is characterized by wheezing, shortness of breath, chest tightness. Globally it affects approximately 300 million people and is estimated to rise to 400 million by 2025 globally [ 1 , 2 ]. And it is ranked 16th among the leading causes of disability and 28th among the leading causes of burden of disease, as measured by disability adjusted life years (DALYs) [ 3 ].
According to Croatian medical journal 2013, an estimate of asthma prevalence in Africa, was 49.7 million in the age of < 15 years (13.9%), < 45 years 102.9 million (13.8%), and in total population 119.3 million (12.8%) in 2010 [ 4 ].
Asthma exacerbation is defined as a worsening of shortness of breath, cough, wheezing, or chest tightness. If not treated immediately there will be increase in flow resistance causing increased work of breathing, gas exchange inefficiency, respiratory muscle tiredness and finally hypercapnic and hypoxemic respiratory failure [ 5 ]. This implies that acute asthma attack is a significant public health problem that affects patients with their parents or families and the community through labor and school loss, frequent emergency clinic visits, a poor quality of life hospitalizations and finally death [ 6 ]. According to Centers for Disease Control and prevention (CDC) report, More than 11 million people reported having an acute asthma attack [ 7 ].
Despite, in Ethiopia little is known about how risk factors are associated with exacerbation, according to asthma severity and the relative importance of the risk factors. This may be the reason for no policy and strategy to ascertain and acting out of effective intervention in order to reduce the burden of acute asthma attack [ 8 ]. Therefore, this study is aimed to full fill this gap.
Study setting and study design
Hospital based unmatched case control study was conducted in the selected general Hospitals of Central zone of Tigray from November 2018 to July 2019.
Study population and sample size determination
Source population.
All adult asthmatic patients visited to emergency unit who have acute asthma attack.
All adult patients diagnosed as asthma but without acute asthmatic attack who visited the OPD and the regular follow-up unit during the data collection period.
Study population
All selected adult asthmatic patients visited to emergency unit who have acute asthma attack during the data collection period.
All selected adult patients diagnosed as asthma but without acute asthmatic attack who visited the OPD and the regular follow-up unit during the data collection period.
Eligibility criteria
Inclusion criteria.
Adult asthmatic patients who have acute asthma attack during the data collection period.
Adult asthmatic patient without acute asthma attack during the data collection period.
Exclusion criteria
Patients with any history of pulmonary embolism, chronic obstructive pulmonary disease, active pulmonary TB, known congestive heart failure and known mechanical obstruction.
Sample size determination
Sample size was calculated from Previous study conducted in Uganda [ 9 ],using Epi info version 7. sample size was determined based on the assumption of confidence level = 95%; Power = 80%; Odds ratio = 2.132 with case to control ratio = 1:2, proportion of among controls 37.2%, proportion of among cases = 55.8%.
Therefore, the required sample size for cases was =92 where as for the controls =183 and the overall sample size was = 275 then after adding 5% non-response rate, the total sample size was 289. Finally, a sample size for cases was 96 and for controls 193.
Sampling technique and procedure
The total sample size was allocated to each hospital proportionally based on the number of patients who attend in the selected hospitals. A total number of 585(case 165, control.420) patients attended at the selected Hospitals with in 2 months of the previous year (April 1 to May 30–2018). Systematic random sampling method was applied in each hospital to select 289 participants.
Study Variables
Dependent variable.
Acute asthma attack.
Independent variables
Socio-demographic variables.
Age, Gender, Marital status, Residence, Educational level, Employment status and Occupational status.
Behavioral factors
Exercise, vigorous activity Smoking cigarette.
Environmental factors
Humidity, Kitchen smoke, dust, Season.
Medical and Clinical characteristics
URTI, Sleep apnea, Missing follow-up / appointments,
Operational definitions
Those who present with cough, wheezing and difficulty of breathing and diagnosed asthma by physician [ 10 ].
Acute Asthma Attack
Those who present with worsening of wheezing, shortness of breath, cough, chest tightness and diagnosed as acute asthma attack by physician [ 10 ].
Smoker:( daily smoker and non-daily smoker) those who currently smokes or those who quit smoking less than 1 year before the assessment [ 10 ].
Passive smoker: Smoke inhaled involuntarily by non-smokers [ 11 ].
Nonsmoker: Respondents who report never smoke those who quit smoking greater than 1 year before the assessment.
Vigorous activity: participants doing activity more than 10 min continuously, that increases breathing, like carrying or lifting heavy loads, digging or construction work, cutting fire wood [ 11 ].
Data collection tool
Structured questionnaire was used to collect the data which was adapted from different literatures [ 9 , 12 , 13 , 14 ]. The questionnaire contains four parts: socio-demographic, environmental factors, behavioral factors, and Medical &Clinical characteristics.
Data collection procedures
Data were collected from cases and controls using structured questionnaire and checklists through face-to-face interview and from patients chart review respectively.
Twelve BSc nurses as data collectors and three senior nurse supervisors were recruited for the data collection, Then data from cases were collected after they take all the necessary medical care and they recover from their attack whereas from the controls data were collected after they have completed their assessment by physician and at the last record reviews from their chart. Participants were identified as having upper respiratory tract infection and Obstructive sleep apnea from their medical charts which was diagnosed by senior physicians. This is to mean that, it was just suspected clinically by the time of the acute event. The reason we obeyed to use clinically diagnosis for obstructive sleep apnea is that, there is no accesses of modern diagnostic modality like polysomnography in the study area which was Tigray regional state not only in the study area but also in the country Ethiopia as a whole. The evaluation protocol that we use were a single evaluation visit for each case and even those who have follow-up and developed acute asthma attack were included .
Data quality control techniques
Data quality was ensured by training of data collectors and supervisors before data collection period. 5% of the questionnaire was pre-tested in Shire Hospital which was not included in the actual data collection. Based on the findings of the pre-test, questionnaire was modified. The filled questionnaire was checked for completeness and accuracy by data collectors, supervisors and principal investigator each day.. The questionnaire was translated into Tigrigna language for better understanding to both the data collectors and respondents and then back translated into English by another expert to ensure accuracy and consistency.
Data analysis procedures
Data were entered in to Epi data version 3.1 and analyzed using SPSS version 23.0. The degree of association between independent and dependent variables were assessed using adjusted odds ratio with 95% confidence interval. Variables < 0.25 p -value in binary logistic regression were entered to multivariable logistic regression model to control the potential confounding variables. Variables with p-value less than 0.05 in multivariable logistic regression model were taken as significantly associated factors. Variance inflation factor (VIF) was used to assess Multicollinearity between the independent variables. Hosmer and Lemeshow goodness fit model were used to check model fitness.
Ethical consideration
Ethical clearance was obtained from Mekelle University College of health sciences institutional review board (IRB). A subsequent permission was also obtained from Tigray teaching hospitals. Respondents were informed about the purpose of the study and the interview was conducted after receiving the written consent from participants. Confidentiality of the data/information was secured and was not used for other purposes.
Sociodemographic characteristic of study participants
Among the participants, 67.7% (65) of the cases and 60.6% (117) of the controls were females. The median ages of participants were 43 years with interquartile range (IQR) of 26.5 years among cases and 43 median ages with interquartile range (IQR) of 22 for control.
The educational status, one third 33.3% (32) of the cases and 24.9% (48) of the controls were collage and above, where as 14.6% (14) of the cases and 16.6% (32) of the controls were unable to read and write. The majority of the cases 63.5% (61) and 60.1% (116) of the controls were married (Table 1 ).
Behavioral characteristics of study participants
Among the participants, 2.1% (2) of the cases and 1.1% (6) of the controls were smokers.in parallel with this 3.1% of the cases and 4.7% of the control were passive smokers. Regarding vigorous activity 37.5% (36) of the cases and 23.8% (46) of the controls were do vigorous activity. Majority of the participants 72.9% (70) of the cases and 58% (112) of the controls were doing exercise.
Medical & clinical characteristics of study participants
Among the participants, 44.8% (43) of the cases and 13.5% (26) of the controls had Upper Respiratory Tract Infections (URTI) and 29.2% (28) of the cases and few of the controls 5.2% (10) had obstructive sleep apnea.
Among the participants, 31.3% (30) of the cases and 20.7% (40) of the controls had Missing follow up.
Environmental characteristics of study participants
Regarding the seasons of a year, spring season (April, May, June) were the season with high percentage 37.7% (109) of acute asthma attack than the autumn season. Majority of the participants 79.5% (230) were open their window/door while they were cooking. Concerning the kitchen of the participants 32.3% (31) of the cases and 20.2% (39) of the control’s kitchen have no kitchen smoke (chimney) (Table 2 ).
Unmatched case control study with 96 cases and 193 controls was conducted to show the determinants of acute asthma attack among adult asthmatic patients visiting general hospitals of central zone, Tigray, Ethiopia.
Having URTI increases the occurrence of acute asthma attack 6.8 times [AOR = 6.835,95% CI = 3.285,14.222] than those who have not upper respiratory tract infection (URTI) (Table 3 ).
This is consistent with the studies conducted in Gondar, Uganda and Ireland [ 9 , 12 , 15 ].
The association might be due to the mechanism of airway inflammation,mucus hyper secretion, and bronchial hyper responsiveness [ 16 ]. In contrast to this study upper respiratory tract infections was no risk factor for acute asthma exacerbation on the study conduct in Pretoria and New Zealand [ 14 , 17 ]. This difference might be due to difference in health care seeking behavior of the participants in this study.
This study revealed that, sleep apnea was strongly associated with the occurrence of acute asthma exacerbation. Those who have sleep apnea are 9.5 times more likely to run in to acute asthma exacerbation than those who have not sleep apnea [AOR = 9.524, 95% CI = 3.563, 25.460].
This findings is comparable with a study done in Gondar and USA [ 12 , 18 ].
The possible reason is the fact that sleep apnea lead to the worsening of asthma control in patients with concomitant sleep apnea secondary to bronchoconstriction as a result of increase vagal tone while sleeping [ 19 ].
The result of this study shows that the odds of having acute asthma in Spring season was 2.2 times higher than the odds of having acute asthma attack in the autumn season [AOR = 2.204,95% CI = 1.011,4.805]. This is consistent with a study conducted in Canada in which spring season was triggering factor for asthma exacerbation [ 20 ]. Seasonal variation is the risk factors for acute asthma attack especially pollens appearing seasons like spring season exacerbates acute asthma attack. This may be due to the reason that during the spring, tree pollen, mold spores and grass have the power to inflame and narrow the air passages of people who have asthma [ 21 ].
The result of this study was different from a study conducted in Spain which was resulting winter season as higher risk of developing acute asthma attack [ 22 ]. The difference could be arisen from seasonal variation between the study areas, due to the influence of temperature and humidity.
In this study, Kitchen smoke (chimney) is highly associated with risk of acute asthma exacerbation.
Those who have no kitchen smoke in their kitchen were 2.3 times at risk to develop acute asthma exacerbation [AOR = 2.307,95%CI = 1.010,5.2725] than those who have kitchen smoke. This finding is comparable with the study conducted in India [ 13 ]. This is due to the fact that kitchen smoke (chimney) is a way that helps in removing the smokes and fumes from the kitchen and making it clean and smoke free which result in reduction of indoor air pollution and prevents acute asthma exacerbation [ 23 ]. Inhaling harmful smoke can inflame lungs and airway, causing them to swell and block oxygen. This can lead to acute asthma exacerbation [ 24 ]
In this study the determinant factors of acute asthma attack were spring season, presence of upper respiratory tract infection (URTI), having no Kitchen smoke in their kitchen and having obstructive sleep apnea.
Limitations
The diagnosis of respiratory tract infections and sleep apnea was empirical (without laboratory) and all measures used were based on self-reporting, this might end up with social desirability bias. This study may have recall bias, since some of the information was based on the recall of the study participants. Unavailability of studies on acute asthma exacerbation.
Availability of data and materials
The datasets used and analyzed during the current study are presented within the manuscript and available from the corresponding author on reasonable request.
Abbreviations
Adjusted Odds Ratio
Confidence Interval
Crude Odds Ratio
Central Statistical Agency
Interquartile Range
National Health Interview Survey
Out Patient Department
Tigray Region Health Development Agency
Upper Respiratory Tract Infection
Variance Inflation Factor
Adams, JY., Sutter, M.E. & Albertson, T.E. The Patient with Asthma in the Emergency Department. Clinic Rev Alleg Immunol 43, 14-29 (2012). https://doi.org/10.1007/s12016-011-8273-z .
Shah R , Saltoun CA . Chapter 14: Acute severe asthma (status asthmaticus). Allergy and Asthma Proceedings, 2012; 33(Supplement 1):S47-S50. Acute severe asthma. InAllergy and Asthma proceedings 2012 (Vol. 33, No. 3, p. 47). OceanSide Publications..
The Global Asthma Report 2018. Auckland, New Zealand: Global Asthma Network, 2018.
Adeloye D, Chan KY, Rudan I, Campbell H. An estimate of asthma prevalence in Africa: a systematic analysis. Croat Med J. 2013;54(6):519–31.
Article Google Scholar
Park HW, Tantisira KG. Genetic signatures of asthma exacerbation. Allergy, Asthma Immunol Res. 2017;9(3):191–9.
Article CAS Google Scholar
Stewart WF, Ricci JA, Chee E, Morganstein D. Lost productive work time costs from health conditions in the United States: results from the American Productivity Audit. J Occup Environ Med. 2003;45(12):1234–46.
CDC , National Health Interview Survey (NHIS) 2014.
Google Scholar
Jackson DJ, Sykes A, Mallia P, Johnston SL. Asthma exacerbations: Origin, effect and prevention. J Allergy Clin Immunol. 2011;128:1165–74.
Sanya RE, Kirenga BJ, Worodria W, Okot-Nwang M. Risk factors for asthma exacerbation in patients presenting to an emergency unit of a national referral hospital in Kampala, Uganda. Afr Health Sci. 2014;14(3):707–15.
Riley L, Gouda H, Cowan M. Noncommunicable Diseases Progress Monitor, 2017: World Health Organization; 2017.
Ethiopia steps report on risk factors for Chronic Non Communicable Diseases and prevalence of selected NCDs. Ethiopia public Health institute. 2016 . .
Belachew SA, Erku DA, Yimenu DK, Gebresillassie BM. Assessment of predictors for acute asthma attack in asthmatic patients visiting an Ethiopian hospital: are the potential factors still a threat? Asthma Res Pract. 2018;4(1):8.
Sharma GL, Choudhary GS. Assessment of Risk Factors for Acute Asthma Attack in Asthmatic Patients: A Hospital Based Study. Int Arch BioMed Clin Res. 2018;4(4):46–8.
Geyser M, Rheeder P. Risk factors precipitating exacerbations in adult asthma patients presenting at Kalafong Hospital, Pretoria. S Afr Fam Pract. 2008;50(4):67–e.
Nicholson KG, Kent J, Ireland DC. Respiratory viruses and exacerbations of asthma in adults. BMJ. 2003;307(6910):982–6.
Fraenkel DJ, Bardin PG, Sanderson G, et al. Lower airways inflammation during rhinovirus colds in normal and in asthmatic subjects. Am J Respir Crit Care Med. 2009;151(3):879–86.
Kolbe J, Fergusson W, Vamos M, Garrett J. Case-control study of severe life-threatening asthma (SLTA) in adults. Thorax. 2002;57(4):317–22.
De-Lei K, Zheng Q, Hui S, Hong Y. Association of Obstructive Sleep Apnea with Asthma exacerbation; 2017.
Alkhalil M, Schulman E, Getsy J. Obstructive sleep apnea syndrome and asthma: what are the links? J Clin Sleep Med. 2009;5(01):71–8.
Tarlo S, Broder I, Corey P, et al. A case-control study of the role of cold symptoms and other historical triggering factors in asthma exacerbations. Can Respir J. 2000;7(1):42–8.
Surrena H, editor. Handbook for Brunner and Suddarth’s textbook of medical-surgical nursing. Lippincott Williams & Wilkins; 2010.
Pola-Bibian B, et al. Asthma exacerbations in a tertiary hospital: clinical features, triggers, and risk factors for hospitalization. J Investig Allergol Clin Immunol. 2016: 0 . https://doi.org/10.18176/jiaci.0128 .
Eisner M, et al. Exposure to indoor combustion and adult asthma outcomes: environmental tobacco smoke, gas stoves, and woodsmoke. Thorax. 2002;57(11):973–8.
Smeltzer SC, Bare BG, Hinkele JL, Cheever KH. Brunner and Suddath’s Text Book of Medical Surgical 2010. Wolters Kluwer Health:Lippincott Williams & Wilkins. Nursing, vol. 1. 12th ed. p. 622.
Download references
Acknowledgments
Authors thanks to public general hospitals of central zone Tigray, Ethiopia for their co-operation, to data collectors, supervisors, for the health staffs of the hospitals and to the study participants for their valuable information.
Not applicable.
Author information
Authors and affiliations.
Department of adult health nursing ,school of Nursing, Aksum University, Aksum, Ethiopia
Melaku Negash & Degena Bahrey Tadesse
Department of Psychiatric, Mekelle University, Mekelle, Ethiopia
Hagos Tsegabrhan
Adwa General Hospital, Adwa, Ethiopia
Teklit Meles
Department of midwifery, Aksum University, Aksum, Ethiopia
Gebreamlak Gidey
college of medicine and health science, Adigrat university, Adigrat, Ethiopia
Yemane Berhane
Maternity and reproductive health nursing, Mekelle University, Mekelle, Ethiopia
Kibrom Berhanu
Department of Emergency and critical care nursing, Mekelle University, Mekelle, Ethiopia
Tsgalem Haylemaryam
You can also search for this author in PubMed Google Scholar
Contributions
MN: was made substantially contributions to conceived and designed the study, analysis the data, methodology, data interpretation and wrote the final manuscript.TM, DB, GG,YB, had equally contributed to analysis and interpretation of the data. Whereas HT, TH and KB substantial contribution in reviewing overall the study in analysis, interpretation of data, have drafted the manuscript and substantively revised the work. All authors read and approved the final manuscript.
Corresponding author
Correspondence to Melaku Negash .
Ethics declarations
Ethics approval and consent to participate.
Ethical clearance was obtained from Mekelle University College of health sciences institutional review board (IRB). Official supportive letters were obtained from Regional Health Bureau (TRHB) and central zone health office. Respondents were informed about the purpose of the study and the interview was conducted after receiving the written consent from participants. The right of participants to withdraw from the study at any time, without any precondition were secured and participants were informed. Confidentiality of the data/information was secured and was not used for other purposes. No personal identifiers was used on the questionnaire. To maintain confidentiality, data collector was recruited from the study unit.
Consent for publication
Competing interests.
The authors declare that they have no competing interests.
Additional information
Publisher’s note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Additional file 1..
Annex I: English version structured interview questionnaire.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/ . The Creative Commons Public Domain Dedication waiver ( http://creativecommons.org/publicdomain/zero/1.0/ ) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
Reprints and permissions

About this article
Cite this article.
Negash, M., Tsegabrhan, H., Meles, T. et al. Determinants of Acute Asthma Attack among adult asthmatic patients visiting hospitals of Tigray, Ethiopia, 2019: case control study. asthma res and pract 6 , 1 (2020). https://doi.org/10.1186/s40733-020-00054-w
Download citation
Received : 07 December 2019
Accepted : 17 March 2020
Published : 03 April 2020
DOI : https://doi.org/10.1186/s40733-020-00054-w
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Acute asthma attack
- Determinants
Asthma Research and Practice
ISSN: 2054-7064
- Submission enquiries: Access here and click Contact Us
- General enquiries: [email protected]

Case of Acute Severe Asthma
Kane guthrie.
- Dec 2, 2022
A 25-year-old lady Miss. Poor Compliance is rushed into your Emergency Department as a Priority 1. She is a brittle asthmatic and has been given 3x 5mg salbutamol nebs, and 0.5mg of adrenaline IM prehospital. On arrival Miss PC is sitting forward in the tripod position , using her accessory muscles to breath. She is tachypnoeic, agitated and unable to talk.
Vital signs: Pulse 143, BP 138/95, RR 42, Sp02 91% on neb, GCS 14/15.
Past Medical and Medication History
- Smoker. Severe asthmatic. Intubated twice in past 2 years
- Currently taking seritide 250/50mg, salbutamol MDI PRN and prednisolone 50mg PRN
Asthma Epidemiology
- Over 2.2 million Australians have currently diagnosed asthma
- 406 deaths attributed to asthma in 2006
- Highest risk of dying from asthma is in the elderly over 70
- The emergency clinician’s goal in treating acute severe asthma is preventing intubation
- Severe/Critical asthma is a life threatening condition
Asthma Pathophysiology
- Asthma is a chronic inflammatory disorder of the airways in which many cells and cellular elements play a role, in particular, mast cells, eosinophils, T lymphocytes, macrophages, neutrophils, and epithelial cells.
- Smooth muscle hypertrophy and hyperplasia
- Inflammatory cell infiltration and oedema
- Goblet cell and mucous gland hyperplasia with mucous hypersecretion
- Protein deposition including collagen
- Epithelial desquamation
- Most common, responsible for 80-85% of all fatal events is characterised by eosinophilic inflammation associated with gradual deterioration over days-weeks occurring in patients with severe or poorly controlled asthma, and is slow to respond to therapy.
- The second phenotype, with neutrophilic inflammation, has both rapid onset and response to therapy.
Markers of severe asthma:
- Inability to speak in full sentences
- Use of accessory muscles or tracheal tugging
- Cyanosis and sweating
- Pulsus paradoxus (>15mmHg decreased with inspiration). With severe muscle fatigue might be absent
- Quiet chest on auscultation (The “Silent Chest”)
- Confusion or decreased level of consciousness
- Hypotension or bradycardia
- FEV 1<40% predicted
- PEF <40% of predicted or best (<25% in life threatening asthma)
- Oxygen saturation <90-92%
- PaO2 <60mmHg
- PaCO2 >45mmHg
Complications of Asthma :
- Pneumothorax, Pneumomediastinum, Pneumopericardium and Pneumoretroperitoneum
- Cardiac Arrhythmias, Myocardial ischaemia or infarction
- Electrolyte disturbances (hypokalaemia, hypomagnesaemia, hypophosphataemia)
- Lactic Acidosis
- Hyperglycaemia
Conditions that may mimic acute asthma:
- Upper airway obstruction
- Foreign-body aspiration
- Vocal cord dysfunction syndrome
- Pulmonary oedema
- Acute exacerbations of COPD
- Hysterical conversion reaction
- Munchausen syndrome
Diagnostic Test:
- Hyperinflation 5-10%
- Infiltrate 5%
- Pneumothorax <1%
- Pneumomediastinum <1%
- Respiratory alkalosis typical
- Inaccurate predictor of outcome
- Will seldom alter your treatment plan
- An objective measure of lung function
- Useful to assess response to treatment
- Impossible to obtain in the dying patient
- <25% Severe
- 25-50% Moderate
- 50-70% Mild
- >70% Discharge Goal
- Simple, and less painful than ABG
- Provides continuous oxygenation measurements
- Needs to placed on well-perfused site, difficult to obtain readings if global hypoperfusion or peripheral vasoconstriction present.
- Aim to keep sp02 >92%
Management of Acute Severe Asthma
- Hypoxia is the main cause of death in asthma
- Oxygen should be given to keep Sp02 above 92%
- A slight Pco2 rise may occur with oxygen therapy but this is of no clinical significance.
Beta-agonists:
- Rapid acting inhaled beta-agonists (bronchodilators) are the first line therapy for acute asthma.
- Nebulisers should generally be used in acute severe asthma, as provide easier delivery of medication to patient, multi dose inhalers have a role in mild to moderate asthma.
- IV salbutamol gives you the advantage of hitting the beta 2 receptors from the back door, while continuing nebulizer treatment, and should be trialed in patients not responding to nebulisers.
- Continuous nebuliser therapy appears to be more effective than intermittent nebulisers for delivering beta-agonist drugs to relieve airway spasm in acute severe asthma. (Cochrane Review, 2009)
- Salbutamol toxicity can caused a lactic acidosis which is often unrecognized in asthma patients, the lactic acidosis has been hypothesized to adversely affect ventilation by increasing ventilatory demand, increasing dead space ventilation, worsening dynamic hyperinflation and intrinsic PEEP. Management is to discontinue salbutamol at the earliest opportunity.
- Dose: Salbutamol Nebuliser Ampoule 5mg
- Dose: Salbutamol IV 5mg in 500mL of 0.9% sodium chloride or 5% dextrose start at 30mL/hr titrating up to 120mL/hr
Anticholinergics:
- Anticholinergics agents block muscarinic receptors in airway smooth muscles, inhibit vagal cholinergic tone and result in bronchodilation.
- Dose: Ipratropium bromide (Atrovent) 500ug to second dose of salbutamol via neb, can be repeated every 4hours
- Use of corticosteroids within 1 hour of presentation to an ED significantly reduces the need for hospital admission in patients with acute asthma. Benefits appear greatest in patients with more severe asthma, and those not currently receiving steroids
- Dose: Prednisolone 50mg PO
- Dose: IV Hydrocortisone 100-200mg
- Note: Parenteral route is indicated in ventilated patient or patient unable to swallow, eg. Vomiting
Adrenaline:
- Can be give either intravenously or via nebulizer
- Bronchoconstriction is the major pathology in asthma; airway oedema might also make a significant contribution. Both the a-agonist and B-agonist effects of adrenaline might be beneficial, with the alpha effect decreasing oedema and the beta effect responsible for bronchodilation.
- Dose: IV 6mg in 100mls 5% dextrose start at 1-15mLs/hour
- Dose: Nebulizer 1mg in 3ml normal saline
Aminophylline:
- The popularity of aminophylline in asthma exacerbations has diminished in recent years.
- Systematic reviews have shown that IV aminophylline in severe acute asthma does not produce additional bronchodilation above that achieved with beta-agonist and corticosteroids.
- Side effects; cardiac arrhythmia’s, vomiting, toxicity.
- Dose : 5mg/kg over 20min followed by infusion of 500mg aminophyline n 500mL of 5% dextrose at 0.5mg/kg per hour
Magnesium Sulphate:
- Magnesium potential role is asthma may involve a combination of smooth muscle relaxation, inhibition of histamine release and acetylcholine release from nerve endings.
- Most evidence to support the use of magnesium in asthma is in the acute severe asthmatic were it has been shown to be safe and beneficial.
- Dose : IV 2-4g over 30-60mins
- Heliox Mixture 80% helium/20% oxygen
- There is evidence that helium and oxygen mixtures (heliox) may provide additional benefits to patients with acute asthma.
- Heliox mixtures have the potential to decrease airway resistance, and therefore decrease the work of breathing for the severe acute asthma patient.
Antibiotics:
- Antibiotics are not indicated in the management of severe acute asthma.
- Antibiotics should only be used in the setting of an underlying pneumonia, respiratory tract infection or to aid in the prevention of ventilator-associated pneumonia in ICU.
Airway Management
Non-Invasive Positive Pressure Ventilation:
Good quality evidence and trails to support the use of NPPV in asthma are lacking, however it is worth trying when intubation is not immediately indicated. Remember the goal of the emergency clinician’s in treating asthma is to prevent intubation.
- Positive pressure is generally less than 15cmH2O
- Benefit between CPAP vs BiPAP is unknown
- Tachypnea caused by severe asthma can make it difficult for the patient to coordinate they’re breathing with machine making BiPAP uncomfortable
- Need a large randomised control trial to determine the effectives properly of NIV, in acute severe asthma.
“Asthmatic on BiPAP before being Intubated”
Mechanical Ventilation:
1-3% of acute severe asthma requires intubation. Prevention of intubation and mechanical ventilation are the goals of managing acute severe asthma, this can be achieved by maximising pre-intubation therapy, however you don’t want to wait too long or let the severe asthmatic tire before trying to intubate them. Once an asthmatic is intubated and ventilated their morbidity and mortality increasing dramatically, and it can be difficult to wean from the ventilator.
Criteria for Intubation:
- Cardiac or Respiratory arrest
- Altered mental status
- Progressive exhaustion
- Severe hypoxia despite maximal oxygen delivery
- Failure to reverse severe respiratory acidosis despite intensive therapy
- pH <7.2, carbon dioxide pressure increasing by more than 5mmHg/hr or greater than 55 to 70mm/Hg, or oxygen pressure of less than 60mm/Hg.
Challenges:
- Effective pre-oxygenation impossible
- No margin for error or delay
- Need to be intubated by most experienced person available
- High intrathoracic pressure after RSI
Recommendations:
- Fluid bolus before intubation if possible
- RSI preferred
- Ketamine for bronchodilator effects
- Permissive hypercapnea essential
Initial Ventilator settings in paralysed patients:
- FiO2 1.0, then titrate to keep SpO2 >94%
- Tidal Volume 5-6ml/kg
- Ventilator rate 6-8 breaths/min
- Long expiratory time (I:E ratio >1:2)
- Minimal PEEP < 5cmH2O
- Limit peak inspiratory pressure to <40cmH2O
- Target plateau pressure <20cmH2O
- Ensure effective humidification
- Brenner, B. Corbridge, T. & Kazzi, A. (2009). Intubation and mechanical ventilation of the asthmatic patient in respiratory failure. The Journal of Emergency Medicine. 37(2s), s23-s34.
- Camargo, C. Rachelefsky, G. & Schatz, M. (2009). Managing Asthma Exacerbation in the Emergency Department: Summary of the National Asthma Education and Prevention Program Expert Panel Report 3 Guidelines for the Management of Asthma Exacerbation.The Journal of Emergency Medicine. 37 (2S), S6-S17.
- Camargo, C. Spooner, C. & Rowe, B. (2009). Continuous versus intermittent beta-agonist for acute asthma (Review). http://www.thecochranelibrary.com.
- Chua, F. & Lai, D. (2007). Acute severe asthma: Triage, treatment and thereafter. Current Anaesthesia & Critical Care. 18, 61-68.
- Creagh-Brown, B. & Ball, J. (2007). An under-recognized complication of treatment of acute severe asthma. American Journal of Emergency Medicine. 26, 513-515.
- Hodder, R. et al. (2009). Management of acute asthma in adults in the emergency department: nonventilatory management. CMAJ. 182(2), E55-E67.
- Holley, A. & Boots, R.(2009). Review article: Management of acute severe and near-fatal asthma. Emergency Medicine Australasia, (21) 259-268.
- Jones, L. & Goodacre, S. (2009). Magnesium sulphate in the treatment of acute asthma: evaluation of current practice in adult emergency departments. Emergency Medicine Journal. 26, 783-785.
- Melnick, E. & Cottral, J. (2010). Current Guidelines for Management of Asthma in the Emergency Department. http://www.ebmedicine.net. 2(2). 1-13.
- Morris, F. & Fletcher, A. (Ed). (2009). ABC of Emergency Differential Diagnosis. Oxford: Blackwell Publishing
- National Asthma Council of Australia. Asthma management handbook: 2006. Accessed http://www.nationalasthma.org.au/cms/images/stories/amh2006_web_5.pdf, 12/02/2010
- Nowak, R. Corbridge, T. & Brenner, B. (2009). Noninvasive Ventilation. The Journal of Emergency Medicine. 37(2S), S18-S22.
- Peters, S. (2007). Continuous Bronchodilator Therapy. Chest. 131(1),1-5.
- Phipps, P. & Garrard, C. (2003). The pulmonary physician in critical care. 12: Acute severe asthma in the intensive care unit. Thorax. 58, 81-88.
- Ram, F. Wellington, S. Rowe, B. & Wedzicha, J. (2009). Non-invasive positive pressure ventilation for treatment of respiratory failure due to severe acute exacerbations of asthma (Review)
- Rodrigo, G. Pollack, C. Rodrigo, C. Rowe, B. (2010). Heliox for non-intubated acute asthma patents (Review).
- Rowe, B. Spooner, C. Ducharme, F. Bretzlaff, J. Bota, G. (2008). Early emergency department treatment of acute asthma with systemic corticosteroids (Review). http://www.thecochranelibrary.com.
- Rowe, B. et al. (2009). Magnesium sulfate for treating exacerbations of acute asthma in the emergency department (Review). http://www.thecochranelibrary.com.
Emergency nurse with ultra-keen interest in the realms of toxicology, sepsis, eLearning and the management of critical care in the Emergency Department | LinkedIn |
Leave a Reply Cancel reply
This site uses Akismet to reduce spam. Learn how your comment data is processed .
- Search Menu
- Sign in through your institution
- Advance Articles
- Supplements
- Author Guidelines
- Reviewer guidelines
- Submission Site
- Open Access
- Self-Archiving Policy
- Why Publish?
- Advertising & Corporate Services
- Advertising
- Reprints and ePrints
- Sponsored Supplements
- Branded Books
- Journals Career Network
- About Paediatrics & Child Health
- About The Canadian Paediatric Society
- Editorial Board
- Journals on Oxford Academic
- Books on Oxford Academic

Article Contents
Case 1 diagnosis: allergy bullying, clinical pearls.
- < Previous
Case 1: A 12-year-old girl with food allergies and an acute asthma exacerbation
- Article contents
- Figures & tables
- Supplementary Data
Lopamudra Das, Michelle GK Ward, Case 1: A 12-year-old girl with food allergies and an acute asthma exacerbation, Paediatrics & Child Health , Volume 19, Issue 2, February 2014, Pages 69–70, https://doi.org/10.1093/pch/19.2.69
- Permissions Icon Permissions
A 12-year-old girl with a history of asthma presented to the emergency department with a three-day history of increased work of breathing, cough and wheezing. She reported no clear trigger for her respiratory symptoms, although she had noted some symptoms of a mild upper respiratory tract infection. With this episode, the patient had been using a short-acting bronchodilator more frequently than she had in the past, without the expected resolution of symptoms.
On the day of presentation, the patient awoke feeling ‘suffocated’ and her mother noted her lips to be blue. In the emergency department, her oxygen saturation was 85% and her respiratory rate was 40 breaths/min. She had significantly increased work of breathing and poor air entry bilaterally to both lung bases, with wheezing in the upper lung zones. She was treated with salbutamol/ipratropium and received intravenous steroids and magnesium sulfate. Her chest x-ray showed hyperinflation and no focal findings.
Her medical history revealed that she was followed by a respirologist for her asthma, had good medication adherence and had not experienced a significant exacerbation for six months. She also had a history of wheezing, dyspnea and pruritis with exposure to peanuts, chickpeas and lentils; she had been prescribed an injectible epinephrine device for this. However, her device had expired at the time of presentation. In the past, her wheezing episodes had been seasonal and related to exposure to grass and pollens; this presentation occurred during the winter. Further history revealed the probable cause of her presentation.
Although reluctant to disclose the information, our patient later revealed that she had been experiencing significant bullying at school, which was primarily related to her food allergies. Three days before her admission, classmates had smeared peanut butter on one of her schoolbooks. She developed pruritis immediately after opening the book and she started wheezing and coughing later that day. This event followed several months of being taunted with peanut products at school. The patient was experiencing low mood and reported new symptoms of anxiety related to school. The review of systems was otherwise negative, with no substance use.
The patient's asthma exacerbation resolved with conventional asthma treatment. Her pulmonary function tests were nonconcerning (forced expiratory volume in 1 s 94% and 99% of predicted) after her recovery. The trigger for her asthma exacerbation was likely multifactorial, related to exposure to the food allergen as well as the upper respiratory infection. A psychologist was consulted to assess the symptoms of anxiety and depression that had occurred as a result of the bullying. During the hospitalization, the medical team contacted the patient's school to provide education on allergy bullying, treatment of severe allergic reactions and its potential for life-threatening reactions with exposure to allergens. The medical team also recommended community resources for further education of students and staff about allergy bullying and its prevention.
Allergy bullying is a form of bullying with potentially severe medical outcomes. In recent years, it has gained increasing notoriety in schools and in the media. Population-based studies have shown that 20% to 35% of children with allergies experience bullying. In many cases (31% in one recent study [ 1 ]), this bullying is related directly to the food allergy. From a medical perspective, there are little published data regarding allergy bullying, and many health care providers may not be aware of the issue.
Allergy bullying can include teasing a child about their allergy, throwing food at a child, or even forcing them to touch or eat allergenic foods. Most episodes of allergy bullying occur at school, and can include episodes perpetrated by teachers and/or staff ( 2 ).
Allergy bullying can lead to allergic reactions, which may be mild or severe (eg, urticaria, wheezing, anaphylaxis), but may also lead to negative emotional consequences (sadness, depression) ( 2 ) and an overall decrease in quality of life measures ( 1 ). Adolescents commonly resist using medical devices, such as injectible epinephrine devices, and bullying may be a contributing factor for this ( 3 ). Attempting to conceal symptoms in a bullying situation may place children at risk for a worse outcome.
Physicians can play a key role in detecting allergy bullying and its health consequences. In many cases, children have not discussed this issue with their parents ( 1 ). Given the prevalence of bullying, its potential to lead to severe harm, including death, and the lack of awareness of this issue, clinicians should specifically ask about bullying in all children and teens with allergies. Physicians can also work with families and schools to support these children, educate their peers and school staff, and help prevent negative health outcomes from allergy bullying.
Online resources
www.anaphylaxis.ca − A national charity that aims to inform, support, educate and advocate for the needs of individuals and families living with anaphylaxis, and to support and participate in research. This website includes education modules for schools and links to local support groups throughout Canada.
www.whyriskit.ca/pages/en/live/bullying.php − A website for teenagers with food allergies; includes a segment that addresses food bullying.
www.foodallergy.org − Contains numerous resources for children and their families, including a significant discussion on bullying and ways to prevent it.
Allergy bullying is common but is often unrecognized as a factor in clinical presentations of allergic reactions.
Physicians should make a point of asking about bullying in patients with allergies and become familiar with resources for dealing with allergy bullying.
Physicians can play roles as advocates, educators and collaborators with the school system to help make the school environment safer for children with allergies who may be at risk for allergy bullying.
Google Scholar
| Month: | Total Views: |
|---|---|
| February 2017 | 2 |
| June 2017 | 2 |
| November 2017 | 3 |
| December 2017 | 6 |
| January 2018 | 3 |
| February 2018 | 5 |
| March 2018 | 7 |
| April 2018 | 10 |
| May 2018 | 8 |
| June 2018 | 13 |
| July 2018 | 3 |
| August 2018 | 5 |
| September 2018 | 8 |
| October 2018 | 6 |
| November 2018 | 8 |
| December 2018 | 22 |
| January 2019 | 1 |
| February 2019 | 8 |
| March 2019 | 3 |
| April 2019 | 13 |
| May 2019 | 9 |
| June 2019 | 5 |
| July 2019 | 17 |
| August 2019 | 12 |
| September 2019 | 15 |
| October 2019 | 6 |
| November 2019 | 3 |
| December 2019 | 4 |
| January 2020 | 8 |
| February 2020 | 10 |
| March 2020 | 16 |
| April 2020 | 44 |
| May 2020 | 65 |
| June 2020 | 102 |
| July 2020 | 119 |
| August 2020 | 104 |
| September 2020 | 221 |
| October 2020 | 286 |
| November 2020 | 391 |
| December 2020 | 336 |
| January 2021 | 456 |
| February 2021 | 492 |
| March 2021 | 661 |
| April 2021 | 646 |
| May 2021 | 662 |
| June 2021 | 507 |
| July 2021 | 389 |
| August 2021 | 484 |
| September 2021 | 628 |
| October 2021 | 860 |
| November 2021 | 752 |
| December 2021 | 627 |
| January 2022 | 599 |
| February 2022 | 698 |
| March 2022 | 922 |
| April 2022 | 913 |
| May 2022 | 728 |
| June 2022 | 450 |
| July 2022 | 299 |
| August 2022 | 406 |
| September 2022 | 668 |
| October 2022 | 956 |
| November 2022 | 915 |
| December 2022 | 771 |
| January 2023 | 649 |
| February 2023 | 707 |
| March 2023 | 769 |
| April 2023 | 646 |
| May 2023 | 748 |
| June 2023 | 428 |
| July 2023 | 356 |
| August 2023 | 387 |
| September 2023 | 567 |
| October 2023 | 743 |
| November 2023 | 691 |
| December 2023 | 524 |
| January 2024 | 493 |
| February 2024 | 667 |
| March 2024 | 743 |
| April 2024 | 767 |
| May 2024 | 750 |
| June 2024 | 333 |
| July 2024 | 143 |
Email alerts
Citing articles via, looking for your next opportunity.
- About Paediatrics & Child Health
- Recommend to Your Librarian
- Advertising and Corporate Services
Affiliations
- Online ISSN 1918-1485
- Print ISSN 1205-7088
- Copyright © 2024 Oxford University Press
- About Oxford Academic
- Publish journals with us
- University press partners
- What we publish
- New features
- Open access
- Institutional account management
- Rights and permissions
- Get help with access
- Accessibility
- Media enquiries
- Oxford University Press
- Oxford Languages
- University of Oxford
Oxford University Press is a department of the University of Oxford. It furthers the University's objective of excellence in research, scholarship, and education by publishing worldwide
- Copyright © 2024 Oxford University Press
- Cookie settings
- Cookie policy
- Privacy policy
- Legal notice
This Feature Is Available To Subscribers Only
Sign In or Create an Account
This PDF is available to Subscribers Only
For full access to this pdf, sign in to an existing account, or purchase an annual subscription.
An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
Preview improvements coming to the PMC website in October 2024. Learn More or Try it out now .
- Advanced Search
- Journal List
- Acad Pathol
- v.7; Jan-Dec 2020
Educational Case: Asthma: Clinical Features and Morphologic Findings
Maria kamal.
1 Department of Pathology, The University of Chicago, IL, USA
Mariam Ghafoor
Urooba nadeem, aliya n. husain.
The following fictional case is intended as a learning tool within the Pathology Competencies for Medical Education (PCME), a set of national standards for teaching pathology. These are divided into three basic competencies: Disease Mechanisms and Processes, Organ System Pathology, and Diagnostic Medicine and Therapeutic Pathology. For additional information, and a full list of learning objectives for all three competencies, see http://journals.sagepub.com/doi/10.1177/2374289517715040 . 1
Primary Objective
Objective: RS4.4: Asthma . Compare and contrast the clinicopathological features and causes of asthma and describe the morphologic changes and consequences that result in airflow obstruction.
Competency 2: Organ System Pathology; Topic: Respiratory System (RS); Learning Goal 4: Obstructive Diseases of the Lung.
Patient Presentation
A 13-year-old male presents to the emergency department with acute onset of breathlessness. He has had recurrent, episodic attacks of wheezing, cough, dyspnea, itchy red eyes, nasal discharge, stuffiness, and occasional chest tightness for past 2 years. Initially, his symptoms were relieved by short-acting β-blocker, albuterol. However, the frequency and the severity of the symptoms have increased for the past 1 month with the patient waking up with these symptoms. He has a history of eczema. His family history is significant for asthma in his mother.
Diagnostic Findings
Physical examination reveals respiratory rate of 22/min and diffuse wheezing all over the lung fields. Pulmonary function test (PFT) shows FEV1/FVC (forced expiratory volume at 1 second [FEV1]/forced ventilatory capacity [FVC]) of 0.65. Forced expiratory volume at 1 second is 60% of predictive and post-bronchodilator therapy the FEV1 increases to 74% of predictive. Chest X-ray is normal.
Question/Discussion Points
What is the diagnosis based on clinical findings and pulmonary function test.
Clinical presentation (recurrent, episodic attacks of wheezing, cough, dyspnea, itchy red eyes, nasal discharge, stuffiness, and chest tightness), and PFT findings (FEV1/FVC of 0.65, FEV1 is 60% of predictive and post-bronchodilator therapy the FEV1 increases to 74% of predictive) are consistent with the diagnosis of asthma. Diagnosis of asthma can be confirmed if the evidence of airway obstruction is seen on PFT, especially if it is reversible with a bronchodilator as seen in our case.
What Type of Lung Disease Is Asthma, and What Are Other Diseases in That Category?
Obstructive diseases of lung are characterized by an increased airflow resistance due to partial or complete obstruction of airway at any level from the trachea to the respiratory bronchioles. In contrast, restrictive diseases show reduced lung parenchymal expansion leading to decreased total lung capacity. Obstructive pulmonary diseases can be distinguished from restrictive diseases based on pulmonary function tests. Obstructive disorders show decreased maximal airflow rates during forced expiration, usually expressed as the FEV1 over the FVC. Obstructive pulmonary diseases generally show a FEV1/FVC ratio of less than 0.7 contrasting with restrictive diseases that are characterized by a proportionate reduction in both total lung capacity and FEV1, resulting in normal FEV1/FVC ratio.
Asthma, emphysema, chronic bronchitis, and bronchiectasis are common obstructive lung diseases. Each has distinct clinical and pathologic characteristics ( Table 1 ). 2 Emphysema and chronic bronchitis are frequently grouped as chronic obstructive pulmonary disease (COPD), as the majority of patients share features of both. Also, both entities are triggered by cigarette smoking. Asthma can be distinguished from COPD by the presence of reversible bronchospasm.
Types of Obstructive Pulmonary Disease.
| Type of obstructive disease | Main pathology | Clinical features | Etiology |
|---|---|---|---|
| Emphysema | Destruction of alveolar walls with minimal inflammation and fibrosis | Progressive dyspnea and cough | Smoking, alpha-1 antitrypsin deficiency |
| Chronic bronchitis | Chronic bronchial inflammation with goblet cell metaplasia and mucous gland hyperplasia | Persistent cough with white to yellow sputum | Smoking, inhaled pollution |
| Asthma | Eosinophilic airway inflammation in majority, basement membrane fibrosis and bronchial smooth muscle hyperplasia | Recurrent but reversible episodes of cough, wheezing and dyspnea | Immune mediated, viral infections, inhaled pollutants, exposure to cold |
| Bronchiectasis | Fixed dilatation of bronchi with fibrosis, and variable acute and chronic inflammation; may be localized or bilateral | Persistent cough with large amount of purulent sputum and recurrent fever | Genetic defects mainly cystic fibrosis, recurrent or severe infection |
What Are the Differential Diagnoses Based on Clinical Findings?
Cystic fibrosis and noncystic fibrosis bronchiectasis.
Both cystic fibrosis (CF) and diffuse non-CF bronchiectasis present with chronic cough and abundant sputum production that is atypical for an asthmatic child. Furthermore, recurrent chest infections are seen in CF patients from a very young age. Patients with non-CF bronchiectasis frequently report productive cough with sputum expectoration, respiratory distress, growth retardation, and night sweats.
Primary ciliary dyskinesia
Primary ciliary dyskinesia (PCD) commonly involves lower airways. It may present as chronic asthma which is usually unresponsive to maintenance therapy. Patients with unexplained respiratory distress at birth and recurrent upper and lower respiratory infections should be screened for PCD.
Protracted bacterial bronchitis
It presents as chronic cough (lasting ≥ 4 weeks) not responding to asthma treatment and require a prolonged (minimum of 2 weeks) course of antibiotic treatment.
Airway foreign body
The sudden onset of respiratory symptoms is more suggestive of an accidental foreign body aspiration than a sudden onset of asthma. It is more common in young children. The patient may present with choking, persistent cough, unilateral and monophonic wheeze, and respiratory distress.
Vocal cord dysfunction
It is characterized by inappropriate adduction of the vocal cords during inspiration induced by exercise, psychological stress, or local irritation like reflux. It frequently coexists with asthma but is unresponsive to bronchodilator therapy. Patients present with breathlessness, intermittent aphonia or dysphonia, choking sensation, chest tightness or pain, difficulty swallowing, and throat clearing. Direct visualization of the vocal cords by endoscopy is the gold standard for the diagnosis. Abnormal shape of the inspiratory loop is seen on spirometry consistent with a variable extrathoracic obstruction.
Bronchiolitis obliterans
Bronchiolitis obliterans occurs secondary to viral and mycoplasma pneumonia infections. It frequently presents as persistent wheezing, rather than paroxysmal symptoms. Computed tomography scan shows a characteristic mosaic pattern and air trapping.
What Is Asthma?
Asthma is a chronic, episodic, inflammatory disorder of the airways associated with bronchoconstriction and airflow limitation that is at least partly reversible, either spontaneously or with treatment. The hallmarks of the disease are as follows 2 :
- ○ Increased airway responsiveness resulting in episodic bronchoconstriction
- ○ Inflammation of the bronchial walls
- ○ Increased mucus secretion
How Does It Present Clinically?
Patients with asthma present with dyspnea, cough, and wheezing due to sudden episodes of bronchospasm. 2 According to the latest National Asthma Education and Prevention Program guidelines, correctly diagnosing asthma is important by establishing the following 3 :
- ○ Episodic symptoms of airflow obstruction or airway hyperresponsiveness
- ○ Airflow obstruction or symptoms are at least partially reversible
- ○ Exclusion of alternative diagnoses.
What Is Acute Severe Asthma (Formerly Known as Status Asthmaticus)?
It is defined as a state of unrelieved attacks of asthma, formerly known as status asthmaticus. It is rare and may prove to be fatal. Usually, it is seen in patients with a long history of severe asthma. Patients may be asymptomatic between episodes. 2
What Are the Risk Factors of Asthma?
Certain factors contribute to the development of airway hyper-reactivity, leading to asthma. These are given as follows 2 :
- ○ Environmental allergens
- ○ Exercise, hyperventilation
- ○ Viral respiratory infections
- ○ Exposure to cold
- ○ Aspirin or nonsteroidal anti-inflammatory drug (NSAID) hypersensitivity
- ○ Inhaled air pollutants such as smoking, sulfur dioxide, ozone, and nitrogen dioxide. Occupational exposure including fumes (epoxy resins, plastics), organic and chemical dusts (wood, cotton, platinum), gases (toluene), or other chemicals (formaldehyde, penicillin products)
What Are the Different Types of Asthma?
Asthma is classified as atopic or non-atopic based on presence or absence of an evidence of allergen sensitization. It may also be categorized according to the triggers that lead to bronchoconstriction. Table 2 shows various types of asthma. 2
Types of Asthma.
| Atopic | Non-atopic | Drug induced | Occupational |
|---|---|---|---|
| – Most common – IgE mediated – Triggered by allergens – Presents in childhood – Positive family history – Diagnosed by RAST (radioallergosorbent tests) | – No evidence of allergen sensitization – Less commonly associated with family history – Triggered by infections (viral commonly) and inhaled air pollutants (SO , ozone, NO ) | – NSAIDs especially Aspirin – Patients present with a triad of rhinitis, nasal polyp and asthma. – Some patients may also develop urticarial. | – IgE mediated – Associated with fumes (epoxy resins, plastics) organic and chemical dust (wood, cotton, platinum) gases (toluene) and other chemicals (formaldehyde and penicillin products) |
Abbreviations: IgE, immunoglobulin E; NSAIDs, nonsteroidal anti-inflammatory drugs.
What Is the Pathogenesis of Asthma?
Asthma results from an interplay between genetic factors, environmental factors, and immune response. Airway inflammation forms the core pathophysiologic mechanism. The pathogenesis of asthma is depicted in Figure 1 . Atopic asthma is characterized by a TH2 and immunoglobulin E (IgE) response to allergens in genetically predisposed individuals. The asthma related genetic polymorphisms possibly influence immune process. Some of the genetic associations are described below 2 :
- ○ Chromosome 5q has a susceptibility locus for asthma close to the gene cluster encoding the cytokines IL-3, IL-4, IL-5, IL-9, and IL-13 and IL-4 receptor among which IL13 gene polymorphisms have the strongest and most consistent association.
- ○ Alleles of class II HLA are associated with production of IgE antibodies against some antigens, like ragweed pollen.
- ○ ADAM33 (a metalloproteinase) gene polymorphisms may be related to increased proliferation of bronchial smooth muscle cells and fibroblasts.
- ○ β2-adrenergic receptor gene variants are linked to differential in vivo airway hyper-responsiveness and in vitro response to β-agonist stimulation.
- ○ IL-4 receptor gene variants are linked to elevated total serum IgE, atopy, and asthma.

Pathogenesis of asthma.
What Are the Morphologic Changes Seen in Asthma?
Gross appearance.
In patients with severe asthma, the lungs appear overinflated showing atelectatic areas. The most prominent gross finding includes airways (bronchi and bronchioles) occluded by thick, tenacious mucus plugs. 2
Microscopic Appearance
A characteristic microscopic finding is Curschmann Spiral ( Figure 2 ) seen in sputum or bronchoalveolar lavage samples of asthma patients. It is the result of mucus plugs extruding from subepithelial mucous gland or bronchioles. Numerous eosinophils with Charcot-Leyden crystals ( composed of an eosinophil protein called galectin-10) are also present. 2 There are other typical microscopic findings of asthma, collectively known as “airway remodeling” that result in airway obstruction, which include ( Figures 3 – 5 ) 2 :

Curschmann spiral (1000×).

Sub-basement membrane fibrosis and submucosal eosinophilic infiltration (×200 magnification).

Squamous metaplasia, sub-basement membrane fibrosis and intraepithelial and submucosal eosinophilic infiltration (×400 magnification).

Goblet cell hyperplasia and smooth muscle hypertrophy (×100 magnification).
- ○ Airway wall thickening
- ○ Subbasement membrane fibrosis (due to type I and III collagen deposition)
- ○ Increase in vascularity and squamous metaplasia
- ○ An increase in the size of the submucosal glands and number of airway goblet cells
- ○ Hypertrophy and/or hyperplasia of the bronchial wall muscle
What Causes Airflow Obstruction in Asthma?
Airflow obstruction is a result of the following changes in asthma 4 :
- Acute bronchoconstriction due to IgE dependent release of mediators (early asthmatic response)
- Airway edema associated with allergen challenge that occurs 6 to 24 hours later (late asthmatic response)
- Exudation of serum proteins and cellular debris resulting in chronic mucus plug formation
- Airway remodeling resulting from structural changes due to chronic inflammation that impacts the extent of airway obstruction reversibility
Airway obstruction leads to increased airflow resistance and expiratory flow rate reduction. These changes result in reduced air expulsion and may lead to hyperinflation of the lung. This overdistention helps preserve airway patency, thus improving expiratory flow. However, it also increases the work of breathing by altering pulmonary mechanics.
Teaching Points
- Asthma results in reversible bronchoconstriction due to hyper-responsiveness of the airway to various stimuli.
- Atopic asthma is the result of an immunologic reaction to environmental allergens and is characterized by acute-phase (immediate) and late-phase reactions.
- Nonatopic asthma has less clear triggers but some viral infections and inhaled air pollutants are known to cause it.
- Almost all subtypes of asthma show eosinophils as key inflammatory cells but other inflammatory cells, for example, mast cells, neutrophils, and T lymphocytes can also be found.
- The irreversible component is the result of extensive airway remodeling (sub-basement membrane fibrosis, bronchial glands hypertrophy, and hyperplasia of smooth muscle).
Declaration of Conflicting Interests: The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding: The author(s) received no financial support for the research, authorship, and/or publication of this article.

Log in using your username and password
- Search More Search for this keyword Advanced search
- Latest content
- Current issue
- BMJ Journals
You are here
- Volume 55, Issue 12
- Case-control study of severe life threatening asthma (SLTA) in adults: demographics, health care, and management of the acute attack
- Article Text
- Article info
- Citation Tools
- Rapid Responses
- Article metrics
- J Kolbe a , b ,
- W Fergusson a ,
- M Vamos c ,
- J Garrett a
- a Department of Respiratory Medicine, Green Lane Hospital, Auckland, New Zealand, b Department of Medicine, University of Auckland, Auckland, New Zealand, c Department of Psychiatry, John Hunter Hospital, Newcastle, NSW, Australia
- Dr J Kolbe, Respiratory Services, Green Lane Hospital, Auckland, New Zealand jkolbe{at}ahsl.co.nz
BACKGROUND Severe life threatening asthma (SLTA) is important in its own right and as a proxy for asthma death. In order to target hospital based intervention strategies to those most likely to benefit, risk factors for SLTA among those admitted to hospital need to be identified. A case-control study was undertaken to determine whether, in comparison with patients admitted to hospital with acute asthma, those with SLTA have different sociodemographic and clinical characteristics, evidence of inadequate ongoing medical care, barriers to health care, or deficiencies in management of the acute attack.
METHODS Seventy seven patients with SLTA were admitted to an intensive care unit (pH 7.17 (0.15), Pa co 2 10.7 (5.0) kPa) and 239 matched controls (by date of index attack) with acute asthma were admitted to general medical wards. A questionnaire was administered 24–48 hours after admission.
RESULTS The risk of SLTA in comparison with other patients admitted with acute asthma increased with age (odds ratio (OR) 1.04/year, 95% CI 1.01 to 1.07) and was less for women (OR 0.36, 95% CI 0.20 to 0.68). These variables were controlled for in all subsequent analyses. There were no differences in other sociodemographic features. Cases were more likely to have experienced a previous SLTA (OR 2.04, 95% CI 1.20 to 3.45) and to have had a hospital admission in the last year (OR 1.86, 95% CI 1.09 to 3.18). There were no differences between cases and controls in terms of indicators of quality of ongoing asthma specific medical care, nor was there evidence of disproportionate barriers to health care. During the index attack cases had more severe asthma at the time of presentation, were less likely to have presented to general practitioners, and were more likely to have called an ambulance or presented to an emergency department. In terms of pharmacological management, those with SLTA were more likely to have been using oral theophylline (OR 2.14, 95% CI 1.35 to 3.68) and less likely to have been using inhaled corticosteroids in the two weeks before the index attack (OR 0.69, 95% CI 0.47 to 0.99). While there was no difference in self-management knowledge or behaviour scores, those with SLTA were more likely to have inappropriately used oral corticosteroids during the acute attack (OR 2.09, 95% CI 1.02 to 4.47).
CONCLUSIONS In comparison with those admitted to hospital with acute severe asthma, patients with SLTA were indistinguishable on sociodemographic criteria (apart from male predominance), were more likely to have had a previous SLTA or hospital admission in the previous year, had similar quality ongoing asthma care, had no evidence of increased physical, economic or other barriers to health care, but had demonstrable deficiencies in the management of the acute index attack. Educational interventions, while not losing sight of the need for good quality ongoing care, should focus on providing individual patients with better advice on self-management of acute exacerbations.
- life threatening asthma
- socioeconomics
- health care
- acute attack
https://doi.org/10.1136/thorax.55.12.1007
Statistics from Altmetric.com
Request permissions.
If you wish to reuse any or all of this article please use the link below which will take you to the Copyright Clearance Center’s RightsLink service. You will be able to get a quick price and instant permission to reuse the content in many different ways.
Read the full text or download the PDF:
- Causes & Prevention
- Symptoms & Types
- Tests & Diagnosis
- Asthma Diet Tips
- Exercising With Asthma
- Living with Asthma: Stress, Anxiety & Depression
- Support & Resources
- View Full Guide
What Causes Asthma? Common Triggers Explained

No one really knows what causes asthma . What we do know is that asthma is a chronic inflammatory disease of the airways. The causes can vary from person to person. Still, one thing is consistent: When airways come into contact with a trigger, they become inflamed, narrow, and fill with mucus.
How Asthma Attacks Happen
When you have an asthma attack, your airways narrow and it gets hard to breathe. This can result from spasms of the muscles around the airways, inflammation and swelling of the mucosal membrane that lines them, or high amounts of mucus inside them. You might have shortness of breath, wheeze or cough as your body tries to get rid of mucus.
Why do you have asthma and your friend doesn't? No one knows for sure. Allergies play a role for many people, as do genetics.
If you or a loved one has asthma, it's important to understand what your triggers are. Once you figure that out, you can take steps to avoid them. As a result, you’ll have fewer and less severe asthma attacks .
Asthma Triggers
Some known triggers of asthma attacks include:
- Food and food additives
- Medications
Allergies Can Cause Asthma
Allergies with asthma is a common problem. Eighty percent of people with asthma have allergies to things in the air, like tree, grass, and weed pollens; mold; animal dander; dust mites ; and cockroach droppings. In one study, children with high levels of cockroach droppings in their homes were four times more likely to have childhood asthma than children with low levels. An allergy to dust mites is another common asthma trigger.
If you have asthma that’s hard to control, see an allergist to find out if you have allergies. Treating your allergies with medication and avoiding your triggers can help lower the odds of a severe asthma attack.
Food and Food Additives Trigger Asthma
Food allergies can cause mild to severe life-threatening reactions. They rarely cause asthma without other symptoms. If you have food allergies , asthma can be part of a severe, life-threatening reaction called anaphylaxis . The most common foods associated with allergic symptoms are:
- Shrimp and other shellfish
- Fresh fruits
Food preservatives can trigger isolated asthma, especially sulfite additives, like sodium bisulfite, potassium bisulfite, sodium metabisulfite, potassium metabisulfite, and sodium sulfite, which are commonly used in food processing or preparation.
Exercise-Induced Asthma
For about 80% of people with asthma, a heavy workout can cause airways to narrow. Exercise is often the main asthma trigger. If you have exercise-induced asthma, you will feel chest tightness, cough , and have trouble breathing within the first 5 to 15 minutes of an aerobic workout. For most people, these symptoms go away in the next 30 to 60 minutes of exercise. But up to 50% of people with exercise-induced asthma may have another attack 6 to 10 hours later. A slow warm-up may help prevent this.
If you have severe asthma and you’re not active now, talk to your doctor first about how to track your breathing and choose the right activities. When it’s winter, avoid exercising outdoors in very cold weather because the exposure could trigger asthma.
Heartburn and Asthma
Severe heartburn and asthma often go hand-in-hand. Up to 89% of people with asthma also have severe heartburn (you might hear your doctor call it gastroesophageal reflux disease, or GERD ). It usually happens at night when you're lying down. Normally, a valve prevents stomach acids from backing up into your esophagus (the tube food goes down when you eat). When you have GERD, this valve doesn't work like it should. Your stomach acids reflux, or back up, into the esophagus. If the acids reach your throat or airways, the irritation and inflammation they cause could trigger an asthma attack.
Clues that suggest reflux as the cause of asthma include the start of asthma in adulthood, no family history of asthma, no history of allergies or bronchitis , difficult-to-control asthma, or coughing while lying down.
If your doctor suspects this problem, they may recommend specific tests to look for it, change your foods, or offer medications .
Smoking and Asthma
People who smoke cigarettes are more likely to get asthma. If you smoke with asthma, it may make symptoms like coughing and wheezing worse. Women who smoke during pregnancy raise the risk of wheezing in their babies. Babies whose mothers smoked during pregnancy also have worse lung function. If you have asthma and you're a smoker, quitting is the most important step you can take to protect your lungs .
Sinusitis and Other Upper Respiratory Infections
Much like asthma causes inflammation in the lining of your airways, sinusitis causes inflammation in the mucus membranes that line your sinuses . This makes the membranes put out more mucus. If you have asthma and your sinuses get inflamed, your airways may too. Prompt treatment of a sinus infection can relieve asthma symptoms.
Infections and Asthma
Cold, flu, bronchitis , and sinus can cause an asthma attack. These respiratory infections that trigger asthma can be viral or bacterial. They're a common cause of asthma, especially in children under age 10. You may be more likely to have an attack for up to 2 months after an upper respiratory infection. Anywhere from 20% to 70% of adults with asthma also have sinus disease. Also, 15% to 56% of people with allergic rhinitis ( hay fever ) or sinusitis also have signs of asthma.
Medications and Asthma
Many people with asthma are sensitive to certain medications that can trigger an asthma attack . If you have asthma , you need to be aware of what other medications may be triggers. You don’t need to avoid these medications unless you know that they’re triggers. But if they have never triggered your asthma , it is still best to take them with caution because a reaction can happen at any time.
Below is a list of the most common medications known to trigger asthma or related symptoms. However, if you are prescribed any medication that you think may be causing your asthma to get worse, discuss it with your doctor.
- Aspirin and other painkillers. About 10% to 20% of people with asthma have sensitivity to aspirin or a group of pain relievers called nonsteroidal anti-inflammatory drugs ( NSAIDs) such as ibuprofen and naproxen . These drugs are often used to treat pain and reduce fevers . Asthma attacks caused by any of these medications can be severe and even fatal, so people who have known aspirin-sensitive asthma should avoid them completely. Products with acetaminophen are generally considered safe for people who have asthma, but you should still talk with your doctor about whether to use them. For some people, there is a small possibility that acetaminophen may trigger an asthma attack. If you have an aspirin sensitivity, it is important that you read the labels of all over-the-counter medications used to treat pain, colds and coughs , and fever. Also, inform your doctor so that these medications are not prescribed for you. If you have any questions about whether a certain medication could trigger your asthma, seek advice from your doctor.
- Beta-blockers. Beta-blockers are commonly prescribed medications used to treat heart conditions, high blood pressure , migraine headache , and, in eye drop form, glaucoma . Your doctor must determine the need for these medications, and you can take a few trial doses to see if they affect your asthma. It is important that you inform all of your health care providers that you have asthma. This includes even your eye doctor. Examples of beta-blockers are Corgard , Inderal , Normodyne , Pindolol , and Trandate .
- ACE inhibitors . These are used to treat heart disease and high blood pressure . These medications can cause coughs in about 10% of the patients who use them. This cough is not necessarily asthma. But it can be confused with asthma or, in the case of unstable airways, can actually trigger wheeze and chest tightness. If you are prescribed an ACE inhibitor and develop a cough , speak with your doctor. Some ACE inhibitors are Accupril , Aceon , Altace , Captopril , Lotensin , Mavik , Monopril , Prinivil , Tarka , Univasc , Vasotec , and Zestril .
If you have severe asthma, talk to your doctor about any medication you’re considering taking, even if it’s an over-the-counter medication. If you know that you're sensitive to particular drugs, make sure your doctor notes the problem on your chart. Always talk to your pharmacist about this reaction before you start a new medication.
Other Asthma Triggers
Irritants. Tobacco smoke, smoke from wood-burning appliances or fireplaces, strong odors from perfumes, cleaning agents, etc., can all trigger asthma. So can air pollution, workplace dust, or fumes from chemicals.
Weather. Cold air, changes in temperature, and humidity can cause an attack.
Strong emotions. Stress and asthma are often seen together. Anxiety, crying, yelling, stress, anger, or laughing hard can bring on an asthma attack.
How Do Triggers Make Asthma Worse?
When you have asthma, your airways are always inflamed and sensitive. They react to a variety of external triggers. Contact with these triggers is what causes asthma symptoms. Your airways tighten and get more inflamed, mucus blocks them, and your symptoms get worse. An asthma attack can start right after exposure to a trigger or several days or even weeks later.
Reactions to asthma triggers are different for each person and vary from time to time. Something may bother you but not others with asthma. You might have many triggers while they have none. And while avoiding triggers is a good way to control asthma, the best way is to take medications and follow treatments exactly as prescribed by your doctor in your asthma action plan.
How Can I Tell What Causes and Triggers My Asthma?
Figuring out what was going on around you when you had an attack is the first step to identifying your triggers.
Your doctor may also do blood testing or ask you to use a device called a peak flow meter. It measures how much air you exhale and how quickly it comes out. It can alert you to changes in your breathing and the onset of asthma symptoms.
Ask your asthma doctor if using a peak flow meter would help you narrow down the causes of your asthma.
It can be tough to identify them all, and they can change. For example, you might not have been bothered by tree pollen when you were a child, only to have a problem with it as an adult.
Even when you know your triggers, you might have a hard time avoiding them in certain situations. For example, you may notice that your workplace is cleaned with a cleaning product that bothers your lungs.
That’s why it’s so important to work closely with the doctor who treats your asthma. They can help you think of strategies to avoid triggers, or at least cut down on the amount of time you spend near them. They can also make sure you have the right medication when an asthma attack does strike.
Know When to Get Help
Warning signs of a potential asthma attack include:
- Needing more rescue inhaler medication (such as albuterol).
- A cough that gets worse.
- Feeling like you can’t breathe or like someone’s sitting on your chest.
- Waking up at night feeling like you can’t breathe.
- Not being able to be active or exercise without getting winded or wheezing.
Use your asthma rescue inhaler medication as soon as you start to feel an attack come on. If it doesn’t seem to work and you feel like you still can’t breathe, call 911 so you can get to an emergency room right away.
If you have a steroid medicine at home (such as prednisone), you can take it on your way to the ER.
- What is Asthma?
- Asthma Attack
- Asthma Causes & Triggers
- Asthma Symptoms
- Asthma Risk Factors
- Types of Asthma
- Diagnosing Asthma
- Asthma Treatment
- Asthma Medications
- Asthma and Anxiety

Top doctors in ,
Find more top doctors on, related links.
- Asthma News
- Asthma Reference
- Asthma Slideshows
- Asthma Quizzes
- Asthma Blogs
- Asthma Videos
- Asthma Community
- Find an Asthma Specialist
- Allergy Relief Advisor
- Cold, Cough & Flu
- Quit-Smoking Assessment
- Lung Disease
- Smoking Cessation
- More Related Topics

IMAGES
VIDEO
COMMENTS
Supported self-management reduces asthma morbidity. The lady in this case study is struggling to maintain control of her asthma within the context of her busy professional and domestic life.
The majority of adverse effects occurred within 1 day of the procedure and resolved within 7 days. 6. In this study, bronchial thermoplasty was found to significantly improve quality of life, as ...
Acute asthma attack is one of the most common causes of visits to hospital emergency departments in all age groups of the population and accounts for the greater part of healthcare burden from the disease. Despite, Acute asthma attack is an important public health problem that affects not only the patients, but also to the family, health professionals, health care institutions and development ...
Case presentation. The patient, a 66-year-old asthmatic man, had a 3-day history of worsening cough, wheeze and shortness of breath that was not relieved by his salbutamol inhaler. ... In a prospective study 7 of 18 patients with acute exacerbation of asthma, attending the emergency department, the change in lactate levels after administering ...
1. INTRODUCTION. Acute severe asthma is a life‐threatening emergency characterized by severe tachypnea, tachycardia, and type 1 respiratory failure. 1 According to the international standard guidelines, it is managed with bronchodilators, systemic steroids, and magnesium sulfate in emergency cases. 2 Here, we describe a case of a 38 years old male who presented with a severe asthmatic attack ...
Severe/Critical asthma is a life threatening condition. Asthma Pathophysiology. Asthma is a chronic inflammatory disorder of the airways in which many cells and cellular elements play a role, in particular, mast cells, eosinophils, T lymphocytes, macrophages, neutrophils, and epithelial cells. The inflammation in asthma cause recurrent episode ...
1. a. Tidal volume is the volume of air inhaled or exhaled during normal quiet breathing. b. Inspiratory reserve volume is the amount of air that can be inhaled after a normal tidal volume. c. Expiratory reserve volume is the amount of air that can be exhaled after a normal tidal volume. How do you think that each of these lung volumes (tidal ...
A 48-year-old female patient with uncontrolled severe asthma was referred to our hospital for anti-IgE therapy. She was suffering with persistent wheezing and dyspnea after a severe asthma attack that had taken place 5 months previously. Her asthma had not been controlled with adequate asthma treatment, including budesonide at 320 μg ...
A therapy with a selective serotonine reuptake inhibitors (Setraline 50 mg b.i.d.) was prescribed. Prednisone could be completely tapered off over 4 weeks. At the end of 10-week pulmonary rehabilitation he reported no relapse of asthma symptoms after cessation of OCS treatment. He seldom needed rescue inhalers, was more fit and had a complete ...
Despite, Acute asthma attack is an important public health problem that affects not only the patients, but also to the family, health professionals, health care institutions and development of the nation, little is known about the risk factors of acute asthma attack. Therefore, this study is aimed to investigate the determinants of acute asthma ...
In recent years, it has gained increasing notoriety in schools and in the media. Population-based studies have shown that 20% to 35% of children with allergies experience bullying. In many cases (31% in one recent study ), this bullying is related directly to the food allergy. From a medical perspective, there are little published data ...
Learning the Asthma Guidelines by Case Studies. Timothy Craig, DO Professor of Medicine and Pediatrics Distinguished Educator Penn State University Hershey Medical Center. Objectives. • 1. Learn the Asthma Guidelines • 2. Be able to classify asthma severity • 3. Be able to determine asthma control • 4. Be able to successfully treat ...
In the present case, PaCO 2 was as high as 90 mmHg at the time of arrival to ED, which was halved and normalized approximately two hours later, consistent with the time course in this study. In this case, we diagnosed asthma as the cause of the cardiac arrest through the background of self-discontinuation of asthma medication, hearing of a very ...
1. Introduction. Asthma is a chronic inflammatory disorder of the airways, a common and potentially serious chronic disease that is associated with variable expiratory flow, airway wall thickening, respiratory symptoms, and exacerbations (flare-ups), which sometimes require hospitalization and may be fatal [].In reference to asthma, an exacerbation is defined as an event characterized by ...
What Is the Diagnosis Based on Clinical Findings and Pulmonary Function Test? Clinical presentation (recurrent, episodic attacks of wheezing, cough, dyspnea, itchy red eyes, nasal discharge, stuffiness, and chest tightness), and PFT findings (FEV1/FVC of 0.65, FEV1 is 60% of predictive and post-bronchodilator therapy the FEV1 increases to 74% of predictive) are consistent with the diagnosis of ...
Attacks often occurred at night or in the early morning. ... A case-control study of deaths from asthma. Thorax 1986;41:833-839. Crossref. PubMed. ISI. Google Scholar. 31. Hogg, JC. The pathology ...
Jane Doe #1. 49 year old female. History of heavy tobacco use and asthma. Patient has been feeling somewhat poorly over the last few weeks and her roommate reports that she has been using her nebulizers quite heavily -despite this, she also has continued to smoke quite heavily. The patient's roommate said that the patient was in her room and ...
Current studies show that Sevoflurane has significant bronchodilator properties and is an effective treatment option for severe acute asthma before rescue therapies [9]. The beneficial effect of Sevoflurane in our case is supported by alveolar unit and distal airway dilation, which reduce distortion of the surrounding parenchyma and amount of ...
A case-control study was undertaken to determine whether, in comparison with patients admitted to hospital with acute asthma, those with SLTA have different sociodemographic and clinical characteristics, evidence of inadequate ongoing medical care, barriers to health care, or deficiencies in management of the acute attack.
The prevalence of asthma in adults in the United States is approximately 7.7%. 1 It is one of the most common chronic, noncommunicable diseases in the country and worldwide. 1,2 Among U.S. adults ...
Cold, flu, bronchitis, and sinus can cause an asthma attack. These respiratory infections that trigger asthma can be viral or bacterial. They're a common cause of asthma, especially in children ...
1 INTRODUCTION. Acute severe asthma is a life-threatening emergency characterized by severe tachypnea, tachycardia, and type 1 respiratory failure. 1 According to the international standard guidelines, it is managed with bronchodilators, systemic steroids, and magnesium sulfate in emergency cases. 2 Here, we describe a case of a 38 years old male who presented with a severe asthmatic attack ...
Asthma is a condition caused by chronic inflammation of the small airways in the lungs. This leads to swelling and increased mucus production within conducting zone pas-sageways. Due to the chronic inflammation, an asthmatic's airways are already more narrow than the airways of an individual without this disease (Figure 1).